Tuberous Sclerosis Complex
Modeling TSC and LAM Using Patient-Derived Induced Pluripotent Stem Cells
Posted May 15, 2018
William L. Stanford, Ph.D., The Ottawa Hospital Research Institute and University of Ottawa

Scientists often study disease by growing cells isolated from patient tissue biopsies. The cells originating from biopsies can be used to understand the basic mechanisms of disease initiation and progression. Furthermore, these cells can be used in drug screens to develop new therapies. However, a major limitation in better understanding tuberous sclerosis complex (TSC) and its associated tumors is that tissue biopsies from TSC patients are rare, particularly from the brain or the lung. Moreover, when biopsies are isolated from TSC patient tumors, scientists have generally been unable to grow the patient cells in culture.
With support from the TSC Research Program, Idea Development Award - Optional Qualified Collaborator, Dr. Stanford, at the University of Ottawa, overcame this limitation by: (1) making stem cells from TSC patient skin cells, and (2) engineering TSC patient mutations in the TSC2 gene into normal stem cells. Using these strategies, he and his team have studied the TSC-related lung tumor called Lymphangioleiomyomatosis (otherwise known as LAM) as well as the cells that contribute to the neurological manifestations of TSC.
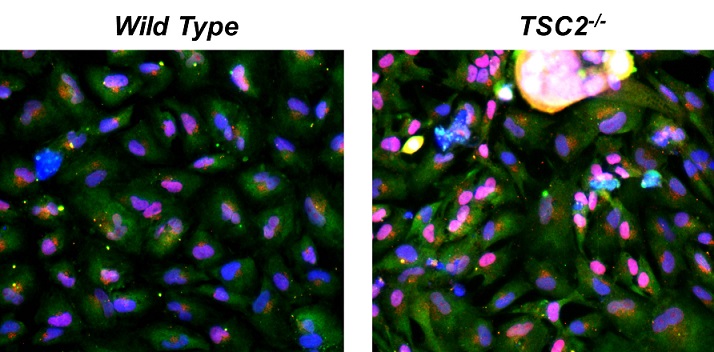
The stem cells Dr. Stanford used in these experiments are pluripotent stem cells, which can differentiate into (become) any of the 240 or so cell types in our body. LAM cells are smooth muscle-like cells; therefore, he allowed the TSC2 mutant stem cells to become smooth muscle cells. As recently published in Cancer Research, the TSC2 mutant smooth muscle cells expressed the same proteins that LAM cells have been shown to express in lung biopsies, demonstrating that these cells can be used to model LAM cells.
Next, Dr. Stanford allowed the TSC2 mutant stem cells to differentiate into neural stem cells, which then differentiated into the three main cell types of the brain. The TSC2 mutant neurons exhibited abnormal shapes and electrical activity. In fact, the abnormal electrical activity of the neurons is similar electrical activity found in epilepsy. Thus, his work showed that he can model both the lung and the neural manifestations of TSC.
In parallel studies, Dr. Stanford developed a material that has many of the same chemical and physical properties of the lung. He grew the TSC2 mutant smooth muscle cells in the lung-like material and has started to perform a drug screen to identify new drugs to kill LAM cells. Similarly, he will seek funding to perform a drug screen on TSC2 mutant neurons to determine whether he can identify drugs to reverse the abnormal electrical activity. He plans to work with clinician scientists to determine which drugs could potentially benefit patients.
In the words of Dr. Stanford: "Our TSC research is an excellent example of the importance of interdisciplinary research in medicine. Our strategy was novel because we used techniques of stem cell biology to address a disease process - in this case, TSC. In doing so, we have learned a lot about TSC from collaborators who treat patients."
Reference:
Julian LM, Delaney SP, Wang Y, Goldberg A, Tam RY, Doré C, Yockell-Lelièvre J, Giannikou G, McMurray F, Harper M-E, Henske EP, Kwiatkowski DJ, Darling TN, Moss J, Shoichet MS, Kristof AS, and Stanford WL. 2017. Human pluripotent stem cell-derived TSC2-haploinsufficient smooth muscle cells recapitulate features of Lymphangioleiomyomatosis. Cancer Research 77:5491-5502.
Link:
Last updated Wednesday, March 19, 2025














