Tuberous Sclerosis Complex
A Novel Model Provides Insight into Tuberous Sclerosis Complex
Posted March 5, 2018
Mustafa Sahin, M.D., Ph.D., Boston Children's Hospital

Tuberous Sclerosis Complex (TSC) is an autosomal dominant disorder that frequently results in tumors, developmental delays, and increased risk for epilepsy and autism spectrum disorder (ASD). Despite the fact that around half of TSC patients go on to develop autism behaviors, the underlying molecular mechanisms connecting TSC and ASD are not well understood. TSC is known to be the result of mutations in the TSC1 or TSC2 genes, but multiple factors, including developmental cerebellar abnormalities, have been implicated in the increased incidence of ASD among TSC patients. While the association between TSC and ASD is recognized among the research community, the absence of critical tools, such as an in vitro model of TSC, has prevented in-depth mechanistic studies, which may lead to a better understanding of the relationship between TSC and ASD and potential novel therapeutics for both.
In 2014, Dr. Sahin was awarded an Idea Development Award to develop an in vitro system to study neurodevelopmental diseases such as TSC. The Sahin lab at Boston Children's Hospital had previously shown that mutation of TSC1 in Purkinje cells in the mouse brain resulted in autism-like behaviors in mice. This preliminary evidence built upon work performed by Dr. Margaret Bauman and others, who identified abnormalities in cerebellar Purkinje cells in ASD patients, leading Dr. Sahin to hypothesize that Purkinje cells were crucial to the underlying molecular mechanisms of TSC and ASD. With support from the Department of Defense Tuberous Sclerosis Complex Research Program, Dr. Sahin used induced pluripotent stem cells (iPSCs) from TSC patients with or without ASD to generate human Purkinje cells in vitro.
Dr. Sahin recently published his findings in the journal Molecular Psychiatry1. Not only did his team successfully develop the first human TSC patient-derived Purkinje cell model, but also showed that the cells were altered in ways comparable to those observed in vivo in the mouse model in both size and activation patterns. TSC2-deficient cells displayed differentiation deficits, increased soma size, autophagy activation, oxidative stress, and cell death. While characterizing the iPSC-derived Purkinje cells, Dr. Sahin's team detected down-regulation of fragile X mental retardation protein (FMRP) as well as synaptic dysfunction and hypoexcitability in cells derived from TSC patients with ASD. Because TSC is a regulator of the mTOR pathway (a series of genes that regulate neural stem cell proliferation), Dr. Sahin decided to investigate the mTOR in-depth in his new in vitro model. As a result, his team determined that the mTORC1 pathway was hyperactivated in TSC patient-derived Purkinje cells. He went on to show that rapamycin, an inhibitor of the mTOR pathway, could partially rescue the TSC patient-derived Purkinje cells' deficits in differentiation, synaptic dysfunction, and hypoexcitability, as well as the downregulation of FMRP.
The limited accessibility to human nervous system tissues up to this point has been a major barrier to TSC and ASD research. Dr. Sahin's in vitro model utilizing human iPSCs will help overcome that barrier and may help to identify and validate novel therapeutic targets, such as the mTOR pathway, for TSC and TSC-associated ASD.
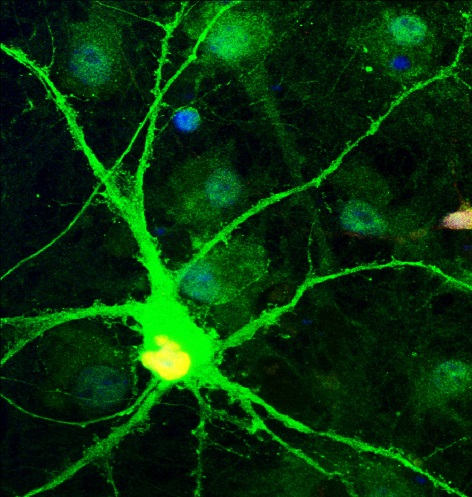
Human Purkinje cell in culture
Reference:
(1) Sundberg M, Tochitsky I, Buchholz DE, Winden K, Kujala V, Kapur K, et al. 2017. Purkinje cells derived from TSC patients display hypoexcitability and synaptic deficits associates with reduced FMRP levels and reversed by Rapamycin. Molecular Psychiatry https://doi.org/10.1038/s41380-018-0018-4.
Link:
Public and Technical Abstracts: Understanding the Role of TSC1/2 in Cerebellar Purkinje Neurons
Last updated Thursday, December 5, 2024














