Spinal Cord Injury
Stentrode: A SCIRP-Funded Device to Facilitate Independence After Paralysis



Posted September 22, 2021
Nicholas Opie, Ph.D., University of Melbourne

Dr. Nicholas Opie holding a
Strentode device in his laboratory.
A Fiscal Year 2016 Spinal Cord Injury Research Program Translational Research Award supported the development and testing of a novel brain-computer interface, the Stentrode, in a large animal model of spinal cord injury. Brain-computer interfaces allow a computer to directly interpret brain signals, such as thoughts, and relay the signals to an output device to carry out an action. The Stentrode (a portmanteau of “stent” and “electrode”) is a thin, flexible neuroprosthesis device,1 implantable within any of the blood vessels in the brain. This method of implantation via the vascular system allows the device to record from the brain without the need for invasive brain surgery, greatly increasing the safety and accessibility of the technology for users. For spinal cord injury, the Stentrode device is implanted within a blood vessel at the top of the head near a section of the brain termed the motor cortex. However, the research team is not limited to implantation at this site and can leverage multiple locations to access different regions of the brain. This means that, in addition to a possible future therapy for spinal cord injury, this technology could potentially be used to address other conditions, such as Parkinson’s disease, epilepsy, post-traumatic stress disorder, and amyotrophic lateral sclerosis (ALS). Researchers at the University of Melbourne, led by Associate Professor Nicholas Opie, used SCIRP funding to refine, manufacture, and perform pre-clinical safety testing of the Stentrode. By the close of the SCIRP award, the Stentrode achieved Food and Drug Administration (FDA)-required benchmarks,2 including those for safety and toxicity. This foundational study was critical for the translation of the device and enabled the initiation of first-in-human clinical testing.
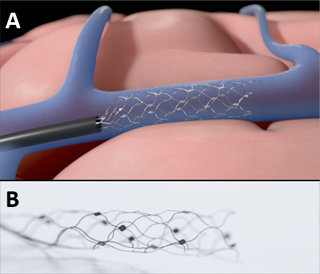
Illustration of Strentrode placement (a) and magnified Strentrode (b).
Following the successful completion of the SCIRP award, the team was ready to move into human clinical testing. The “Stentrode First in Human Early Feasibility Study” (SWITCH, NCT03834857), an industry-funded clinical trial, initiated in Melbourne, Australia. To date, the study enrolled four participants with severe paralysis due to ALS-associated motor deficits.3 After only minimal training with the Stentrode interface, participants learned to use eye movements and thoughts to control a computer cursor and keyboard. As simple as it sounds, these computer controls allow the participants to autonomously perform many activities of daily living once believed impossible, such as composing an email, using a smart phone to communicate via text message, or purchasing a gift online for their significant other. The Stentrode enabled these participants to regain their ability to independently communicate with the world around them, something one participant had been unable to do for 4 years. This first clinical study does not just provide proof of concept for this technology, but also gives real hope for individuals living with neurological disorders or injuries to regain meaningful independence and autonomy. These achievements are vital to improving psychosocial wellness and quality of life in individuals living with paralysis.
In July 2021, the FDA granted Investigational Device Exemption approval for the Stentrode, paving the way for an early feasibility trial in the U.S. The COMMAND trial at Mount Sinai Hospital in New York, is expected to begin late 2021 (supported by the National Institutes of Health Brain Initiative,5 Stentrode manufacturer Synchron, and venture capital funding).

Stentrode development and testing was supported through a broad network of federal and non-governmental funding enties.
References:
1 Oxley TJ, Opie NL, John SE, et al. 2016. Minimally invasive endovascular stent-electrode array for high-fidelity, chronic recordings of cortical neural activity. Nat Biotechnol. Mar;34(3):320-327. doi: 10.1038/nbt.3428. Epub 2016 Feb 8. PMID: 26854476.
2 Opie NL, Rind GS, John SE, et al. 2016. Feasibility of a chronic, minimally invasive endovascular neural interface. Ann Int Conf IEEE Eng Med Biol Soc. Aug;4455-4458. doi: 10.1109/EMBC.2016.7591716. PMID: 28269267.
3 Oxley TJ, Yoo PE, Rind GS, et al. 2021. Motor neuroprosthesis implanted with neurointerventional surgery improves capacity for activities of daily living tasks in severe paralysis: First in-human experience. J Neurointerv Surg. Feb;13(2):102-108. doi: 10.1136/neurintsurg-2020-016862. Epub 2020 Oct 28. PMID: 33115813; PMCID: PMC7848062.
4 https://www.businesswire.com/news/home/20210728005305/en
Link:
Last updated Friday, December 19, 2025
 An official website of the United States government
An official website of the United States government
 ) or https:// means you've safely connected to the .mil website. Share sensitive information only on official, secure websites.
) or https:// means you've safely connected to the .mil website. Share sensitive information only on official, secure websites.
