Peer Reviewed Orthopaedic



Posted January 20, 2023
Dustin R. Grooms, Ph.D., AT, CSCS, Ohio University

(Photo provided)
Musculoskeletal injury to the anterior cruciate ligament (ACL) often leads to impaired performance, which current surgical reconstruction and physical therapy may not always fully restore. These injuries are common in the civilian and military populations, with high rates of reinjury and long recovery times. Current rehabilitation methods tend to focus on mechanical milestones relating to knee motion and load, but data on the impact of the central nervous system on recovery are limited. Dr. Dustin Grooms and key co-investigators, Dr. Janet Simon and Dr. Brian Clark, from Ohio University are quantifying brain activity in high-risk and ACL injury-repaired individuals to help identify the regions affected and develop new rehabilitation strategies.
Dr. Grooms was awarded a fiscal year 2017 Peer Reviewed Orthopaedic Research Program (PRORP) Applied Research Award to determine the neuroplasticity associated with ACL injury/therapy, and what functional correlates exist to be viable targets for intervention. In other words, this study is assessing how certain regions in the brain change after ACL injury across the typical 6-month window of physical therapy, using new functional evaluations to target the brain changes that may limit performance and recovery. The overall goal of the project is to add to the body of knowledge regarding cognitive-visual-motor integration after injury. The team is also incorporating virtual reality (VR) during the recovery process to stimulate a complex environment to help reduce reinjury. This VR environment is designed to promote proper motor control and minimize the cognitive resources to control the knee.
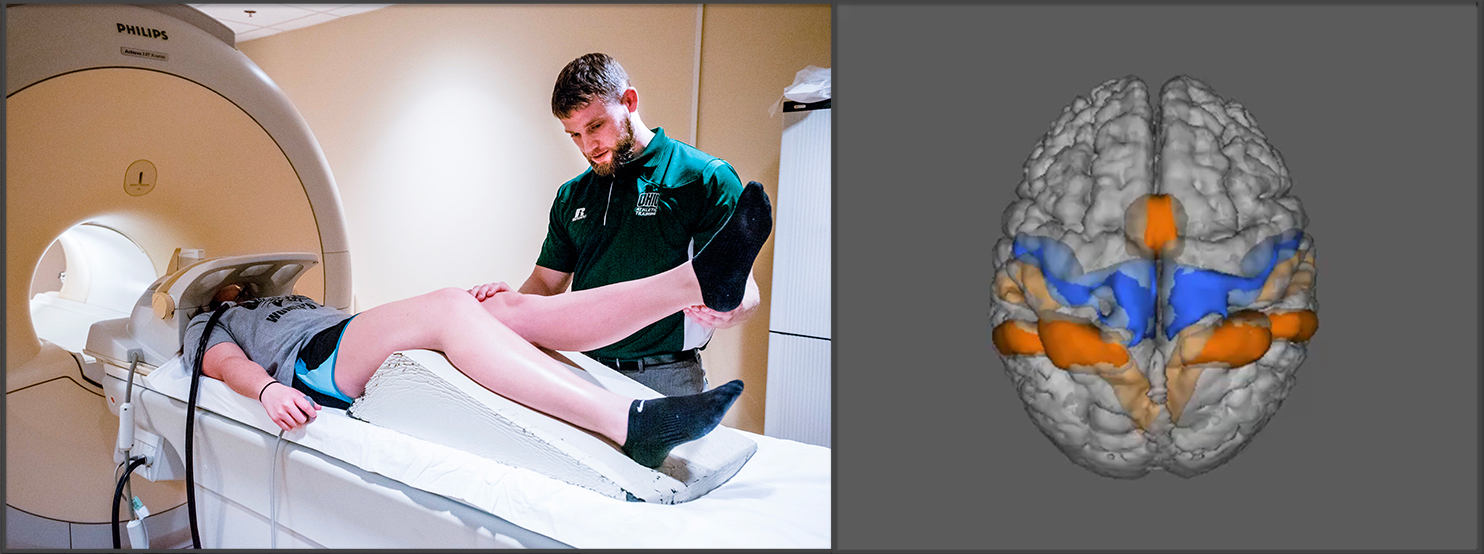 Figure 1: (left) One of the fMRI knee motor tasks used in the ACL-reconstruction cohort to identify the brain activation pattern for knee motor control after injury. (right) The knee motor control brain activation of those with high ACL injury risk (orange).
Figure 1: (left) One of the fMRI knee motor tasks used in the ACL-reconstruction cohort to identify the brain activation pattern for knee motor control after injury. (right) The knee motor control brain activation of those with high ACL injury risk (orange).
Dr. Groom' PRORP-funded project has produced several publications on topics quantifying neural activity for knee motor control, identifying brain activity in persons with high versus low risk of ACL injury, and investigating how cognitive motor interference and virtual reality affects motor function in athletes and Reserve Officer' Training Corps (ROTC) research volunteers. His team has used functional MRI (fMRI) to identify specific neural paradigms to quantify lower extremity neuromuscular function (Figure 1).1 This technique has now been incorporated into evaluating female high school athletes with high versus low risk of ACL injury by assessing the motor control brain activity between the two groups. Their findings suggest that elevated brain activity in specific regions of the brain is associated with a higher risk of injury.2 Additionally,
 Figure 2: (left) ROTC study volunteer engaging the cognitive-motor inference simulated shooting task using laser rifle range. (right) Athletic return to sport cognitive-motor interference testing.
Figure 2: (left) ROTC study volunteer engaging the cognitive-motor inference simulated shooting task using laser rifle range. (right) Athletic return to sport cognitive-motor interference testing.
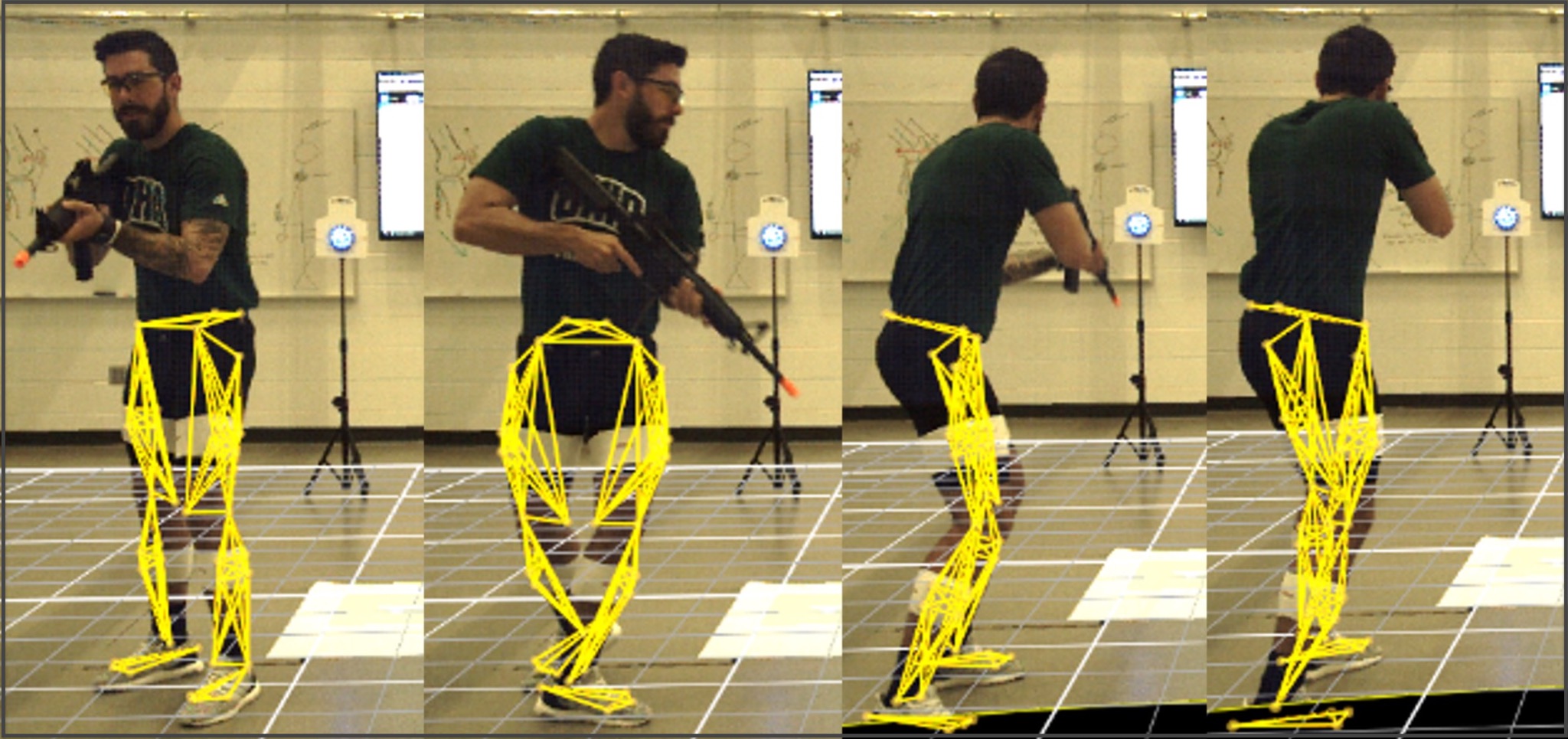 Figure 3: ROTC study volunteer engaging in cognitive-motor interference shooting trial instrumented to capture lower extremity biomechanics (outlined in yellow).
Figure 3: ROTC study volunteer engaging in cognitive-motor interference shooting trial instrumented to capture lower extremity biomechanics (outlined in yellow).
Throughout his past and current work, Dr. Grooms has been able to demonstrate the importance of cognitive function in physical rehabilitation. He has now demonstrated the benefits of incorporating environment and cognitive load in training tools for increased performance and injury prevention.
References:
1Grooms DR, Criss R, Simon JE, et al. 2021. Neural correlates of knee extension and flexion force control: A kinetically instrumented neuroimaging study. Frontiers in Human Neuroscience 14, 622637. https://doi.org/10.3389/fnhum.2020.622637
2Grooms DR, Diekfuss JA, Criss CR, et al. 2022. Preliminary brain-behavioral neural correlates of anterior cruciate ligament injury risk landing biomechanics using a novel bilateral leg press neuroimaging paradigm. PLOS One 17(8):e0272578. https://doi.org/10.1371/journal.pone.0272578
3Buckley S, Chaput M, Simon JE, et al. 2022. Cognitive load impairs time to initiate and complete shooting tasks in ROTC members. Military Medicine 187(7-8), e898:e905. https://doi.org/10.1093/milmed/usab276
4Brazalovich P, Simon JE, Criss CR, et al. 2022. The effects of virtual reality immersion on drop landing mechanics. Sports Biomechanics. Published online February 9. https://www.tandfonline.com/doi/full/10.1080/14763141.2022.2035427
5Farraye BT, Chaput M, Simon JE, et al. 2022. Development and reliability of a visual-cognitive medial side hop for return to sport testing. Physical Therapy in Sport 57:40-45. https://doi.org/10.1016/j.ptsp.2022.07.004
Last updated Sunday, December 31, 1600
 An official website of the United States government
An official website of the United States government
 ) or https:// means you've safely connected to the .mil website. Share sensitive information only on official, secure websites.
) or https:// means you've safely connected to the .mil website. Share sensitive information only on official, secure websites.
