Peer Reviewed Orthopaedic
Development of Large Animal Models for Improved Regenerative Therapies in Bone Healing and Volumetric Muscle Loss Injury



Posted April 13, 2021
Todd McKinley, M.D., Melissa Kacena, Ph.D., Indiana University

Traumatic musculoskeletal and extremity injuries are pervasive in combat settings and contribute significantly to long-term disability and medical discharge of wounded Service Members.1 Of specific concern are type III open fractures involving severe bone and soft-tissue injury that result in segmental bone defects (SBD) and volumetric muscle loss (VML). VML is an injury in which large pieces of muscle are lost or removed, such as injuries that result from explosive blast trauma, and account for more than 90% of muscle conditions in battlefield-injured Service Members who are medically retired.1,2 These complex musculoskeletal injuries are a major challenge in orthopaedic care and often require focused orthopaedic fracture repair through multiple surgical interventions in which bone union can be difficult to achieve and restoration of muscle function is unproven. Approximately one quarter of lower-limb open fractures result in non-union which results in additional surgeries and significant morbidity, and can ultimately lead to loss of extremity function.3 Combinations of autogenous bone grafts, biodegradable scaffolds with bone morphogenetic protein 2 (BMP‐2), an osteoinductive growth factor, are often used to improve healing in large bone defects. However, autografts are limited by defect size. Additionally, BMP-2 has been associated with adverse effects, including heterotopic bone formation, which could require additional surgeries. Even with successful bone healing, chronic functional deficits often persist due to the concurrently traumatized muscle tissue resulting from VML injury and contribute to low quality of life, limb amputation, and military medical discharge.
There is no definitive clinical standard of care for regeneration of lost muscle tissue in VML injuries. Current treatment options include traditional rehabilitative therapies, such as physical therapy, and have limited benefit toward functional recovery.2 Due to the high incidence of VML injury among wounded Service Members and limited treatment options, the Peer Reviewed Orthopaedic Research Program (PRORP) is committed to the development of novel regenerative therapies with solutions that can properly address these challenging musculoskeletal injuries for accelerated healing timelines of complex fractures and therapeutic enhancement of muscle regeneration. With a Fiscal Year 2012 (FY12) PRORP Translational Research Partnership Award, Drs. Melissa Kacena and Todd McKinley, along with their research team at Indiana University, investigated whether thrombopoietin (TPO), a megakaryocyte growth factor that improves bone healing, is efficacious and safer than BMP-2 for bone regeneration in critical-sized tibial defects in a large animal model. The research team developed a large-animal model of open fracture by creating 25- (metacritical-sized) or 40- (critical-sized) millimeter (mm) bone defects in the mid-shaft of right hind limbs of minipigs; removed the resulting free segment of bone; and filled the defect sites with scaffolds surrounded by type I collagen sponges soaked with either TPO, BMP-2, or saline. The 25 mm defects were stabilized with intramedullary nails and with dual plating (open reduction and internal fixation [ORIF]). The 40 mm defects were stabilized with ORIF. The most significant findings during this period demonstrated that in pigs with 25 mm defects, those treated with ORIF healed and those treated with intramedullary nailing fixation did not heal. Furthermore, all pigs with a 40 mm defect treated with saline failed to heal. Addition of BMP-2 resulted in successful healing in all 25 and 40 mm defects. Finally, TPO treatment improved healing compared to saline treated controls, but was not as robust or consistent at BMP-2 treatment. TPO-treated animals did not display adverse effects from blood analyses, organ pathology, or veterinary inspection. Overall, these results are supportive of the efficacy and safety of TPO for bone healing in large animals, though additional optimization of dosing or timing of drug treatment were still needed.
Dr. McKinley and his team continued to expand their work and performed extensive studies investigating regenerative therapies for skeletal muscle injury specific to VML. Preclinical studies from this group demonstrate that severe muscle trauma impairs endogenous healing as well as recombinant human BMP-2 mediated fracture healing in rodent models of open fracture. The research team determined that VML results in dysregulated muscle inflammation that spreads to the nearby fracture callus and delays the inflammatory phase necessary for fracture healing. Moreover, the team reported that use of autologous minced muscle grafts, which are pieces of the donor’s own muscle with optimized biomaterials, improved bone and muscle healing through rescued fracture healing, as well as dampening of the local immune responses and promoted muscle tissue regeneration.
Through additional funding from an FY16 PRORP Applied Research Award, Dr. McKinley and his team are expanding upon their original minipig model of open fracture to represent impaired fracture healing with concomitant VML injury. Dr. McKinley will further establish the role of severe muscle trauma inflammation in the healing impairment of non-critical-sized, endogenously healing tibial defects. The research team also sought to determine whether autologous minced muscle grafts could rescue fracture healing and restore the functional capacity of the traumatized musculature. In the minipig model, the research team is employing a 25-mm segmental bone defect treated with dual plating (ORIF) that leads to delayed bone healing along with an adjacent volumetric muscle defect in the anterior compartment of the lower limbs. Dr. McKinley hypothesized that using a minced skeletal muscle autograft (SMA) to repair severely traumatized skeletal muscle subjected to an SBD combined with VML will modulate the local wound environment and result in rescued fracture healing and restoration of muscle form and function.
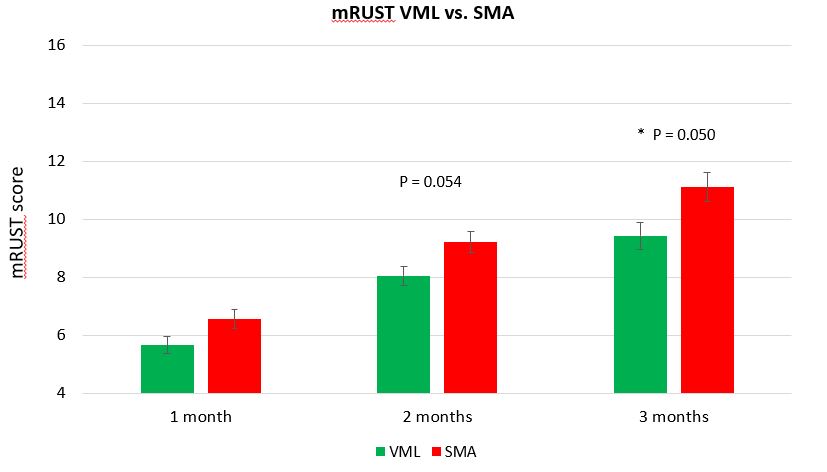
Figure 1. Overall, modified Radiographic Union Score for Tibia fractures (mRUST) scores for specimens with a segmental bone defect and an untreated volumetric muscle defect (VML) versus specimens with a segmental bone defect and volumetric muscle defect filled with skeletal muscle autograft (SMA). At the time of sacrifice (three months after injury) SMA animals had improved bone healing, as indicated by higher mRUST scores.
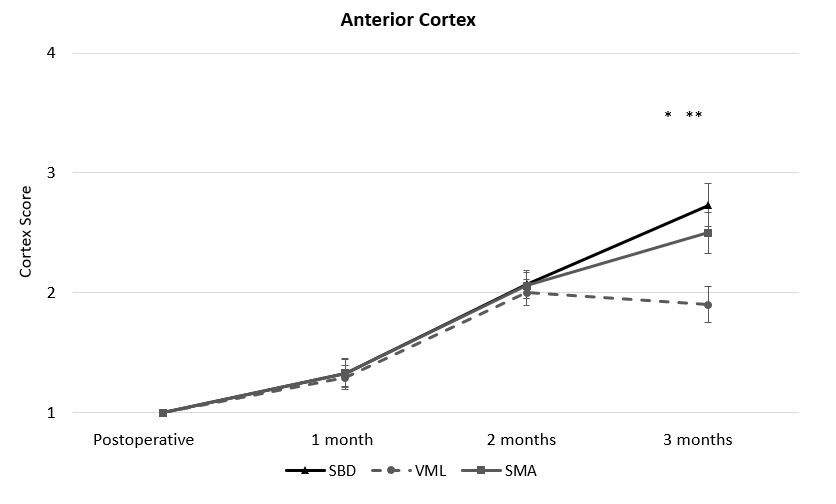
Figure 2. The improvements in bone healing resulting from muscle autografting (SMA specimens) were primarily measured in the anterior cortex which was immediately adjacent to the muscle defect and grafted region. Muscle autografting (SMA) restored anterior cortex healing to the level of animals with an isolated segmental bone defect and no muscle injury (SBD). Both SMA (*) and SBD (**) specimens had significantly improved mRUST scores for the anterior cortex compared to specimens with untreated muscle defects (VML).
The most recent results of this work demonstrate that SMA improved the overall bone healing in minipigs with VML defects at two and three months after injury (Figure 1). Bone healing was quantified by modified Radiographic Union Score for Tibia fractures (mRUST) and confirmed with computerized tomography scanning. Overall, mRUST scores in pigs with muscle defects filled with SMA trended higher at two months (P = 0.054) and were significantly increased at three months (P = 0.050) compared to pigs with unfilled volumetric muscle defects (VML). Specifically, bone healing improvements in the anterior cortex immediately adjacent to the muscle graft were the most pronounced (Figure 2). However, muscle function was not restored by muscle grafting. Interestingly, muscle strength deficits at three months were equal among pigs that either had an isolated segmental bone defect with no muscle injury (SBD), a muscle defect that was untreated (VML), and a VML defect treated with skeletal muscle autografting (SMA) (Figure 3). These results demonstrated the magnitude of a bone defect, which had an overwhelming effect on local muscle function. The investigators are expanding this work to investigate methods to stage and pre-treat VML defects to improve muscle function in future experiments. Results from this novel large animal model of VML could establish efficacy of muscle grafting in a preclinical model, which would support rapid translation into human use and provide the foundation for innovative regenerative therapies to advance the standard of care for musculoskeletal trauma involving VML injury and improve healing outcomes.
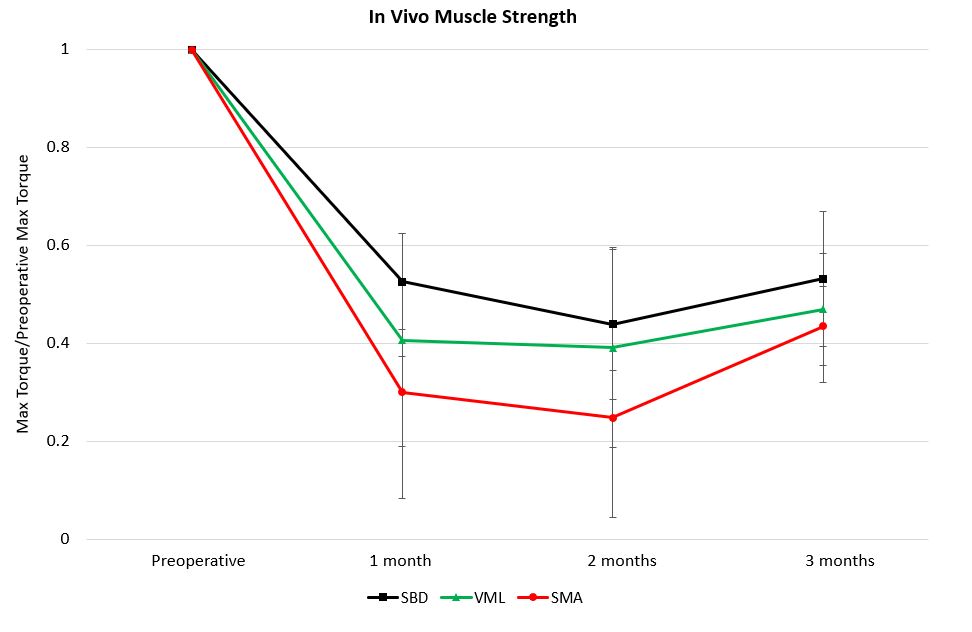
Figure 3. At the time of sacrifice, three months after injury, muscle autografting (SMA) did not improve in vivo muscle strength in the anterior compartment of the leg compared to animals with untreated muscle defects (VML). Interestingly, the data demonstrate that the presence of the bone defect had the most significant effect on muscle function as animals with isolated bone defects and no muscle injury (SBD) had similar in vivo strength compared to VML and SMA animals. These data highlight the effect of bone injury on adjacent muscle function.
With support from the PRORP, Dr. McKinley and his research team are addressing a significant extremity injury among Service Members to fill a significant unmet clinical need in orthopaedic care. The team is further advancing therapies for clinical translation through follow-on funding from an FY19 Peer Reviewed Medical Research Program Investigator-Initiated Research Award to develop and optimize a multi-staged regenerative approach for VML that could be utilized in conjunction with current clinical approaches for enhancing bone fracture healing. Dr. McKinley’s research, if successful, has the potential for rapid clinical translation and could significantly impact treatment of complex musculoskeletal injuries to improve the overall quality of life of wounded Service Members.
Publications:
McKinley TO, Natoli RM, Fischer JP, Rytlewski JD, Scofield DC, Usmani R, Kuzma A, Griffin KS, Jewell E, Childress P, and Shively KD. 2020. Internal fixation construct and defect size affect healing of a translational porcine diaphyseal tibial segmental bone defect. Military Medicine.
Davis KM, Griffin KS, Chu TG, Wenke JC, Corona BT, McKinley TO, and Kacena MA. 2015. Muscle-bone interactions during fracture healing. Journal of Musculoskeletal and Neuronal Interactions15(1):1.
Griffin KS, Davis KM, McKinley TO, Anglen JO, Chu TMG, Boerckel JD, and Kacena MA. 2015. Evolution of bone grafting: bone grafts and tissue engineering strategies for vascularized bone regeneration. Clinical Reviews In Bone And Mineral Metabolism13(4):232-244.
Jewell E, Rytlewski J, Anglen JO, McKinley TO, Shively KD, Chu TMG, and Kacena MA. 2015. Surgical fixation hardware for regeneration of long bone segmental defects: translating large animal model and human experiences. Clinical Reviews in Bone and Mineral Metabolism13(4):222-231.
References:
- Corona BT, Rivera JC, Owens JG, Wenke JC, and Rathbone CR. Volumetric muscle loss leads to permanent disability following extremity trauma. Journal of Rehabilitation Research & Development 52(7).
- Greising SM, Corona BT, McGann C, Frankum JK, and Warren GL. Therapeutic approaches for volumetric muscle loss injury: A systematic review and meta-analysis. Tissue Engineering Part B: Reviews 25(6):510-525.
- Harris AM, Althausen PL, Kellam J, Bosse MJ, Castillo R. Lower Extremity Assessment Project (LEAP) study group. Complications following limb-threatening lower extremity trauma. Journal of Orthopaedic Trauma23(1):1-6.
Links:
Public and Technical Abstracts: Novel Therapy for Bone Regeneration in Large Segmental Defects
*In conducting research using animals, the investigator(s) adheres to the laws of the United States and regulations of the Department of Agriculture.
Last updated Wednesday, September 17, 2025
 An official website of the United States government
An official website of the United States government
 ) or https:// means you've safely connected to the .mil website. Share sensitive information only on official, secure websites.
) or https:// means you've safely connected to the .mil website. Share sensitive information only on official, secure websites.
