Peer Reviewed Orthopaedic
Development of a High-Performance, Adaptable Prosthetic Socket for Amputees



Posted August 22, 2017
Jason Wheeler, Ph.D., Sandia National Laboratories

Sandia National Laboratories
There are nearly 2 million Americans living with the loss of a limb. Amputation represents a major care concern for the Armed Forces; with more than 1,500 major limb amputations in military personnel serving in Afghanistan and Iraq. Unfortunately, despite improvements to overall function of modern prosthetics, the fit and comfort of the prosthetic limb are often the deciding factors in prosthetic use or abandonment. The residual limb is a dynamic tissue that experiences volume and shape changes throughout the day, as the body accommodates to different activities. Furthermore, the residual limb volume changes over time in response to muscle and weight fluctuations. These challenges are magnified in above the knee amputees, who lack both the ankle and knee joint required for ambulation. These patients frequently experience a stiff, awkward, and inefficient gait as well as skin irritation at the prosthetic site. The challenge of maintaining a good prosthetic fit is complicated by a lack of diagnostic tools to monitor the interface between the limb and the socket over time or during physical activity. Additionally, current prosthetics are limited in their ability to provide fundamental functions of the foot, such as appropriately distributing loads throughout the residual limb and giving sensory feedback to the wearer. Thus, there is a need to develop a socket that can track and adapt to changes in residual limb dynamics, as well as provide force and joint position feedback to the user. Such a socket would improve the comfort and functionality of the prosthetic, particularly for people who want to maintain an active lifestyle.
With support from an FY2009 Peer Reviewed Orthopaedic Research Program (PRORP) Technology Development Award, Dr. Jason Wheeler and his team at Sandia National Laboratories have addressed specific issues in the maintenance or enhancement of long-term socket performance and the fit of prosthetic devices for both above and below the knee amputees. Lower-limb prosthetic sockets are made of two components: a hard-shell exterior for stability, and a soft, flexible, internal liner for limb adhesion to the device and comfort. The three goals of Dr. Wheeler's work were to develop a socket liner that could monitor the volume and shape changes of the residual limb, adapt to these changes in real time, and provide sensory feedback to the wearer regarding joint position and prosthetic movement. In order to track changes in the residual limb, Dr. Wheeler and his team developed a novel sensor embedded within a silicone liner that could measure normal and shear pressures from three different directions: (1) pressure pushed into the skin (normal), and pressures that run (2) up/down or (3) side-to-side along the surface of the skin (shear). This new technology represents an exciting new capability not available in other sensor systems. By collecting pressure changes during various forms of movement or activity through the use of this novel liner, clinicians would be able to monitor their patients for potential issues, such as excessive rubbing that could lead to blisters or abrasions, and recommend adjustments to the socket fit. Dissemination of such technology could greatly improve the ability of clinicians to spot fit problems before problematic skin irritations develop and help patients maximize the use of their prosthetics. Taking this work a step further, Dr. Wheeler also incorporated a system of bladders, or channels, into the liner that can alter their fluid volume in response to changes in residual limb size or shape, as detected by the pressure sensors. Preliminary tests with patients found that the liner adjusted well to changes in limb volume during laboratory use and was comfortable to wear.
Refinement and development of Dr. Wheeler's sensory and adaptive socket liner as it moves toward clinical availability is ongoing, with increased patient testing (in collaboration with Dr. Joan Sanders at the University of Washington) and improved manufacturing of the device to transition the sensor system to market for use with multiple prosthetics. Thus far, two United States Patents have been granted as a result of Dr. Wheeler's research in developing this liner, and several additional patent applications have been submitted. Stemming from the success of this project, Dr. Wheeler has also been able to conduct further exploratory studies to develop a system that can utilize tactile feedback to provide above-the-knee amputees information to reduce their reliance on vision for basic tasks like walking or climbing stairs. This work is still in the early stages, but has generated promising results such as improved walking confidence in test subjects.
As the number of amputees in the United States continues to grow, with projections of citizens living with limb loss reaching 3.6 million by 2050, the need for improved and comfortable prosthetic sockets, particularly for above the knee amputees, remains an unmet medical issue. The sensory measurements collected by Dr. Wheeler's liner will provide clinicians with quantitative and reliable data to ensure the best socket fit for their patients. Additionally, people with above the knee amputations will greatly benefit from the improved function and comfort of the adaptive liner as they seek to maintain an active lifestyle.

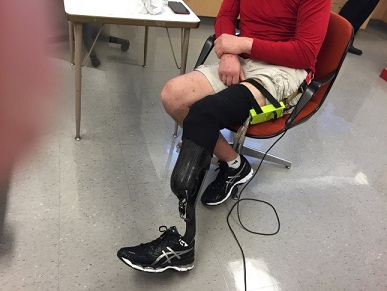
Right image: User with instrumented socket liner and prosthetic of choice.
Publications:
Wheeler, J., Mazumdar, A., Marron, L., Dullea, K., Sanders, J., Allyn, K., "A Pressure and Shear Sensing Liner for Prosthetic Sockets," in IEEE Engineering in Medicine and Medicine and Biology Society Annual Conference, Orlando, FL, 2016.
Lincoln LS, Quigley M, Rohrer B, Salisbury C, and Wheeler JW. 2012. An Optical 3D force sensor for biomedical devices. 4th IEEE International Conference on Biomedical Robotics and Biomechatronics, Rome, Italy.
Dabling JG, Filatov A, and Wheeler JW. 2012. Static and cyclic performance evaluation of sensors for human interface pressure measurement. 34th International Conference of IEEE EMBS, San Diego, California.
Lincoln LS, Bamberg SJM, Parson E, Salisbury C, and Wheeler JW. 2012. An Elastomeric Insole for 3-Axis Ground Reaction Force Measurement. 4th IEEE International Conference on Biomedical Robotics and Biomechatronics, Rome, Italy.
Sanders JE, Cagle JC, Harrison DS, Myers TR, and Allyn KJ. 2013. How Does Adding and Removing Liquid from Socket Bladders Affect Residual Limb Fluid Volume? Journal of Rehabilitation Research and Development. 50(6)845-860.
Patents:
Skin Stretch Tactile Feedback Device. US Patent number 8491665 (granted 7/23/2013).
Optical based tactile shear and normal load sensor. US Patent Number 9052775 (granted 6/9/2015)
Links:
Video from Sandia National Laboratories where Dr. Wheeler explains the sensory liner:
https://www.youtube.com/watch?v=iSd9m16dux0
News Release on shear force sensor development:
https://share-ng.sandia.gov/news/resources/news_releases/prosthesic_sensor/#.WZb1d7pFwRB
Last updated Wednesday, March 12, 2025














