Peer Reviewed Medical
Strain-Programmable Bioadhesive Patch for Accelerated Healing of Diabetic Ulcer


Posted August 23, 2023
Xuanhe Zhao, Ph.D., Massachusetts Institute of Technology
Aristidis Veves, D.Sc., M.D., Beth Israel Deaconess Medical Center
Eleven percent of Americans, and almost a quarter of the American Veteran population, have been found to struggle with diabetes.1,2 Insulin, a hormone released by the pancreas that allows sugar or glucose created after digestion to be used by cells for energy, does not properly function in diabetes and cannot adequately regulate blood sugar levels. This dysfunction can lead to long-term medical issues, affecting areas such as vision, organ disease, and wound healing.3 Diabetic patients experience impaired wound healing that limits quality of life, commonly in the form of diabetic foot ulcers (DFUs). Research into inducing healing in DFUs has proven difficult, referencing the need for existing wound dressings to contribute actively to the treatment and closure of the wound, beyond its passive role as a wound covering.
Between fiscal years 2015-2022 (FY15-FY22), Congress included Diabetes as a Peer Reviewed Medical research Program (PRMRP) Topic Area. With an FY20 PRMRP Investigator-Initiated Research Award - Partnering PI (Principal Investigator) Option, Drs. Xuanhe Zhao and Aristidis Veves have been designing and testing the potential of a new wound dressing to treat DFUs and other wounds in the form of a strain-programmable bioadhesive patch. The patch works with forces of strain, or tension, along the skin to pull the wound edges closer together for more efficient healing, to improve adherence to the skin, and to outperform current commercially available alternatives. The patch's use of two layers with different properties plays a crucial role in increasing its capabilities. The inner bioadhesive layer absorbs fluids from the wound and contracts in a programmable manner to allow for mechanical modulation of the underlying wound, while the outer layer remains flexible and provides protection from the external environment.
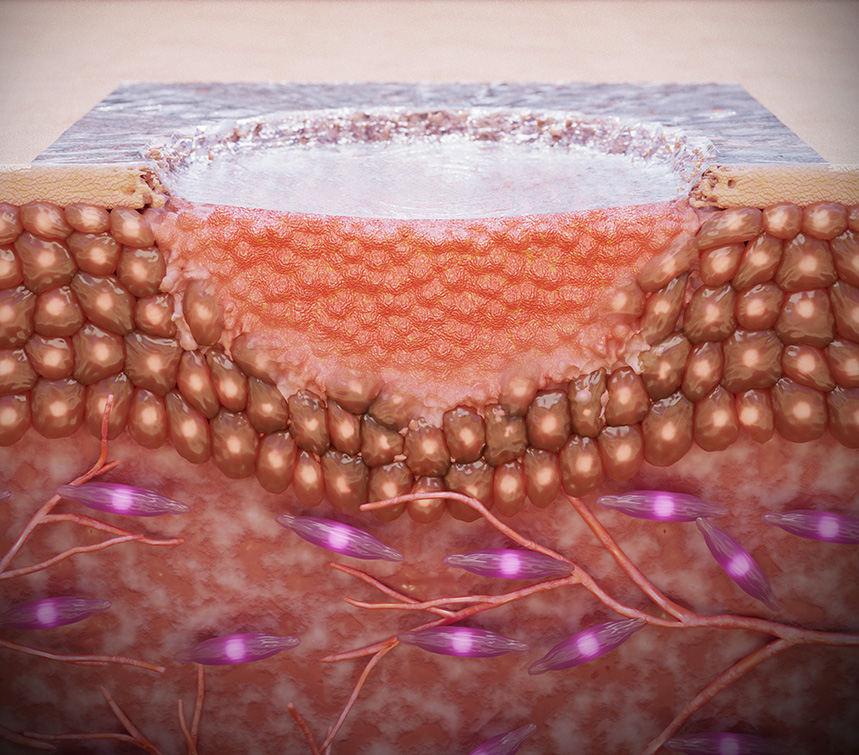
The investigators evaluated the strain-programmable bioadhesive patch's proposed performance through a series of mechanical tests that assessed the durability of the patch, its wound closure strength, and its strain programming and adhesion capabilities. They also tested the ability of the patch to promote wound healing in diabetic mouse and pig models. The team found the patch could promote diabetic wound healing in acute conditions, or treatment of a newer wound that has not yet begun to heal. They also found the patch to be capable of promoting healing in chronic conditions or in treatment of a wound with preexisting tension due to improper healing. Evaluation of the patch in the pig model showed a capability to account for differences in wound shape, suggesting it has the potential to treat more difficult wound cases. The researchers demonstrated that the patch facilitated better wound repair by accelerating the formation of new epidermis, fostering the growth of blood vessels, and stimulating pro-regenerative cell types.
As Drs. Zhao and Veves prepare to transition their bioadhesive patches to the clinic, they plan to comprehensively map the molecular processes impacted by the application of the patch and understand the processes involved in the repeated application or exposure to this treatment. They also recently filed for a patent covering this discovery and licensed it for potential commercialization to a spinoff startup, SanaHeal, located in Boston. Overall, this strain-programmable bioadhesive patch has broad significance in treatment for diabetic patients and potential future implications in wound care for other conditions.
 Dr. Xuanhe Zhao, from the Massachusetts Institute of Technology, and
Dr. Xuanhe Zhao, from the Massachusetts Institute of Technology, and
References:
1Centers for Disease Control and Prevention. National Diabetes Statistics Report. https://www.cdc.gov/diabetes/php/data-research/index.html .
2Liu Y, Sayam S, Shao X, et al. 2017. Prevalence of and Trends in Diabetes Among Veterans, United States, 2005-2014. Centers for Disease Control and Prevention. Preventing Chronic Disease 14:E315. https://doi.org/10.5888/pcd14.170230 .
3Centers for Disease Control and Prevention. What is Diabetes? https://www.cdc.gov/diabetes/about/index.html.
Publications:
Theocharidis G, Yuk H, Roh H, et al. 2022. A strain-programmed patch for the healing of diabetic wounds. Nature Biomedical Engineering 6:1118-1133. "https://doi.org/10.1038/s41551-022-00905-2
Links:
Last updated Friday, December 19, 2025
 An official website of the United States government
An official website of the United States government
 ) or https:// means you've safely connected to the .mil website. Share sensitive information only on official, secure websites.
) or https:// means you've safely connected to the .mil website. Share sensitive information only on official, secure websites.
