Peer Reviewed Cancer
Novel Targets for the Treatment of Metastatic Colorectal Cancer



Posted April 21, 2023
Dr. Daniel V. LaBarbera, Ph.D., University of Colorado Anschutz Medical Campus
 Dr. Daniel V. LaBarbera
Dr. Daniel V. LaBarbera
(Photo Provided)
Colorectal cancer (CRC) is the third most prominent cancer in the U.S. and the second leading cause of cancer-related death, according to the National Institutes of Health (NIH) National Cancer Institute (NCI). Epithelial-mesenchymal transition (EMT) is a behavioral change in cancer cells that contributes to the transition of CRC into metastatic CRC (mCRC). During EMT, tumor cells transition from an anchored state to a mobile state with increased ability to invade other tissues and body sites and may also develop multi-drug resistance. T-cell factor (TCF) transcription is a modulator of the EMT pathway. TOP2A is a protein that regulates TCF and, therefore, has an impact on EMT and disease progression. Current drugs that target TOP2A work by causing DNA damage, and this can have significant side effects, including hair loss and sickness. As indicated by the NCI, 5-year survival rates for patients diagnosed with late-stage and metastatic colorectal cancer (mCRC) are low, at approximately 15%, demonstrating a need for new treatments to improve patient quality of life and outcomes.
With a fiscal year 2012 (FY12) Peer Reviewed Cancer Research Program (PRCRP) Career Development Award, Dr. Daniel LaBarbera and his team sought to identify new treatments that revert the EMT process to treat mCRC. The team identified a naturally occurring compound, neoamphimedine (neo), that inhibits TOP2A and works differently than TOP2A poisons, presumably with less side effects. They designed and synthesized derivatives of neo to enhance its stability and impart better drug-like properties. They then assessed anti-tumor activity in the lab and confirmed that the neo derivates inhibit growth and promote cell death in three-dimensional tumor cell cultures, called organoids, due to inhibition of EMT.
After determining which neo derivatives worked best individually on tumor organoids, the team planned to study the derivatives' combined effect with known cancer drugs.
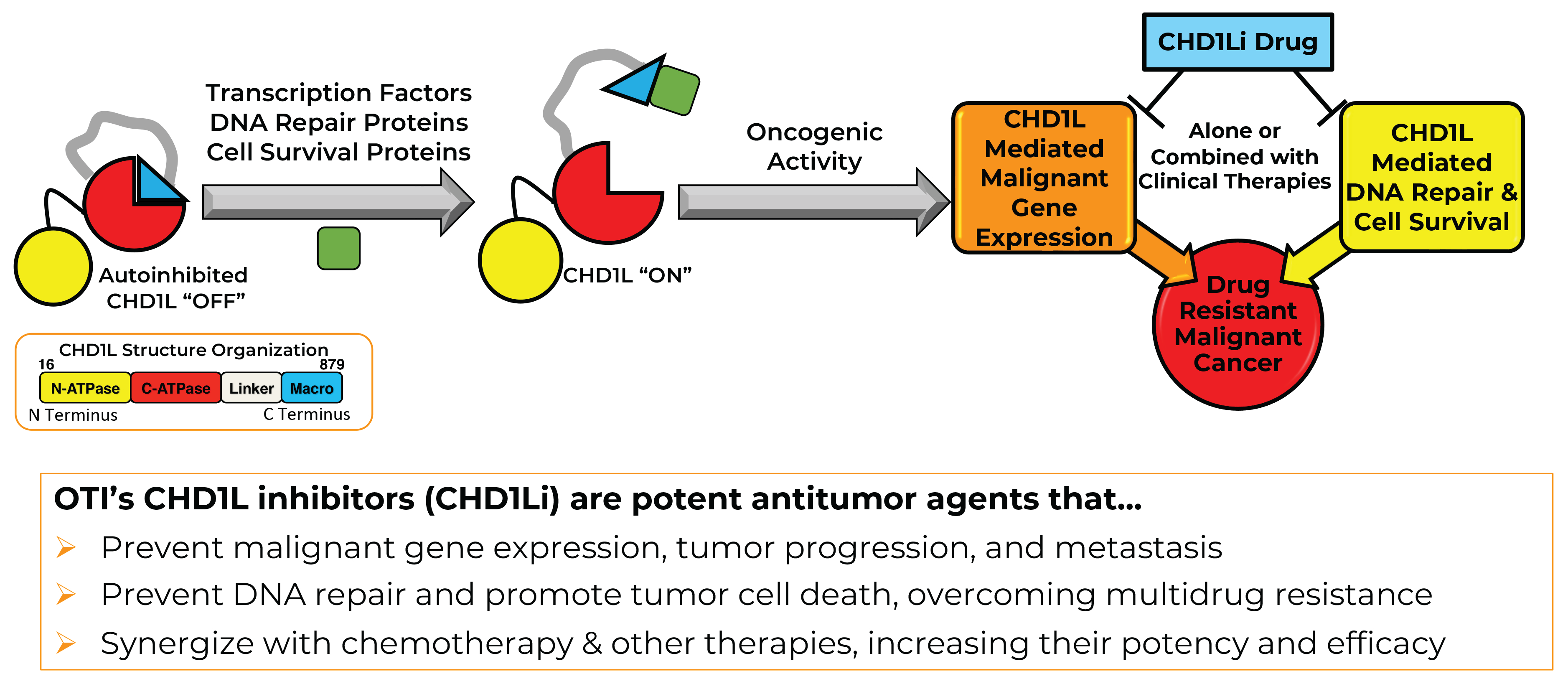
Fig. 1. Schematic of oncogenic CHD1L and CHD1Li antitumor action. CHD1L is a chromatin remodeler that has N-(yellow) and C-(red) terminal ATPase lobes. CHD1L is unique from other chromatin remodelers because it contains the C-terminal macro domain (blue) that functions as a molecular switch rendering it catalytically "on" or "off." In normal cells or cells that are non-dividing or proliferating, the CHD1L macro domain autoinhibits itself. However, CHD1L is amplified or overexpressed in tumor cells. CHD1L is recruited by proteins and transcription factors driving tumor progression and survival via binding of the macro domain (green square), turning on CHD1L-mediated gene expression, EMT, DNA repair, and cell survival. CHD1Li are effective antitumor agents alone and strongly synergize with chemotherapy and targeted therapies. (Figure Provided)
Next, Dr. LaBarbera's team identified small-molecule inhibitors of CHDL1 (CHD1Li), including lead CHD1Li 6.0, and studied its activity in a variety of in vitro and in vivo models of CRC (Fig 1). CHD1Li 6.0 reverses EMT in tumor organoids, ultimately resulting in death of the tumor cells, and inhibits migration and invasion of human CRC cell lines in laboratory studies.
With the eventual goal of using CHD1Li 6 for human CRC therapy, the team studied its effect in combination with several chemotherapeutic drugs. Many of these drugs cause death in cancer cells by inducing DNA damage. The research team tested combination treatment of CRC cell lines with CHD1Li 6 and Irinotecan/SN-38, a chemotherapeutic used in the treatment of CRC. The combined treatment synergizes to induced greater DNA damage in the cells than SN-38 alone, indicating CHD1Li 6 may enhance the effectiveness of DNA-damaging chemotherapy if successfully translated to patient treatment. To verify its activity and begin testing safety,
Subsequent work funded by the NIH NCI (1R01CA251361) focused on medicinal chemistry optimization of the pharmacophore of CHD1Li 6.0 led to the development of a pipeline of novel CHD1Li 6.0 analogs. This work has led to a cancer drug pharmaceutical startup company, Onconaut Therapeutics Incorporated (OTI), founded by Dr. LaBarbera in 2022. OTI is developing the first- and best-in-class lead drugs targeting CHD1L, with several lead clinical candidates at the technology readiness Level (TRL) between TRL3 (proof of concept achieved), TRL4 (demonstrate in vivo efficacy and safety), and TRL5 (FDA Investigational New Drug [IND]-enabling studies).
Dr. LaBarbera's research serves as the groundwork for future studies of EMT-targeting therapies that could provide new treatment options for people living with CRC. This work also successfully identified new therapeutic strategies to target regulators of EMT in order to mediate drug resistance and metastases in CRC and could be applied to the treatment of other cancers. In particular, OTI is focused on translating CHD1Li to the clinic for public use and benefit for the treatment of CRC and other types of cancers.
Dr. LaBarbera and his team have also developed a dual-reporter tool for the evaluation of EMT by assessing two differentially expressed proteins on cancer cells before and after transition. This tool could be valuable for other cancer researchers who want to study the effect of new therapies on EMT.
References:
Colorectal Cancer-Patient Version. (n.d.). National Cancer Institute. Retrieved February 17, 2023, from https://www.cancer.gov/types/colorectal.
Cancer Stat Facts- Colorectal Cancer. (n.d.). National Cancer Institute. Retrieved February 17, 2023, from https://seer.cancer.gov/statfacts/html/colorect.html.
Publications:
Abraham AD, Esquer H, Zhou, Q, et al. 2019. Drug design targeting T-cell factor-driven epithelial-mesenchymal transition as a therapeutic strategy for colorectal cancer. Journal of Medicinal Chemistry 62(22):10182-10203. https://doi.org/10.1021/acs.jmedchem.9b01065.
Abbott JM, Zhou, Q, Esquer H, et al. 2020. First-in-class inhibitors of oncogenic CHD1L with preclinical activity against colorectal cancer. Molecular Cancer Therapeutics 19(8):1598-1612. https://doi.org/10.1158/1535-7163.MCT-20-0106.
Esquer H, Zhou Q, Nemkov T, et al. 2021. Isolating and targeting the real-time plasticity and malignant properties of epithelial-mesenchymal transition in cancer. Oncogene 40(16):2884-2897. https://doi.org/10.1038/s41388-021-01728-2.
Links:
Last updated Monday, December 15, 2025
 An official website of the United States government
An official website of the United States government
 ) or https:// means you've safely connected to the .mil website. Share sensitive information only on official, secure websites.
) or https:// means you've safely connected to the .mil website. Share sensitive information only on official, secure websites.
