Psychological Health/Traumatic Brain Injury
Is telemedicine-delivered therapy as effective as treatment delivered at the clinic?
Posted March 22, 2016
Ron Acierno, Ph.D.; VA Medical Center in Charleston
 The prevalence of post-traumatic stress disorder (PTSD) is high among service members returning from Operation Enduring Freedom and Operation Iraqi Freedom (OEF/OIF), and many experience debilitating conditions that can end military careers. Accumulating evidence for exposure based therapies and behavioral activation based interventions show effectiveness in reducing the symptoms of PTSD and depression; however, these therapies remain inaccessible or impractical for a large number of Servicemen and women in need. Administering these therapies requires well-trained clinicians and it is often difficult and costly to maintain this staff at facilities spread across the country. Servicemen and women seeking treatment also face the investment of time and money to travel to treatment centers for repeated sessions, as well as the risk of stigma related to visiting a mental health facility. These and other hurdles often lead participants to drop out of treatment, leaving the effectiveness of these evidence-based therapies limited by high attrition rates. Advances in telemedicine delivery of therapy have the potential to overcome these hurdles by providing remote audio-visual conferencing between provider and patient, ultimately increasing access by making sessions easier to attend. However, it must first be established that telemedicine based delivery of these therapies is as effective as treatment in person.
The prevalence of post-traumatic stress disorder (PTSD) is high among service members returning from Operation Enduring Freedom and Operation Iraqi Freedom (OEF/OIF), and many experience debilitating conditions that can end military careers. Accumulating evidence for exposure based therapies and behavioral activation based interventions show effectiveness in reducing the symptoms of PTSD and depression; however, these therapies remain inaccessible or impractical for a large number of Servicemen and women in need. Administering these therapies requires well-trained clinicians and it is often difficult and costly to maintain this staff at facilities spread across the country. Servicemen and women seeking treatment also face the investment of time and money to travel to treatment centers for repeated sessions, as well as the risk of stigma related to visiting a mental health facility. These and other hurdles often lead participants to drop out of treatment, leaving the effectiveness of these evidence-based therapies limited by high attrition rates. Advances in telemedicine delivery of therapy have the potential to overcome these hurdles by providing remote audio-visual conferencing between provider and patient, ultimately increasing access by making sessions easier to attend. However, it must first be established that telemedicine based delivery of these therapies is as effective as treatment in person.
Through work funded by a 2007 Department of Defense (DoD) PTSD Investigator-Initiated Research Award, Dr. Ron Acierno and his team at the Charleston Research Institute, the Ralph H. Johnson VA Medical Center, and the Medical University of South Carolina, compared the effectiveness of delivering a treatment for PTSD and depression directly into patients' homes to the identical treatment delivered at a clinic. One hundred ninety-six (196) Servicemen and women from OEF/OIF (as well as the Gulf War and Vietnam War) who had been diagnosed with PTSD were randomized to receive eight sessions of behavioral activation and therapeutic exposure (BA-TE) therapy either in person or at home via telemedicine delivery. Participants were then assessed for symptoms of PTSD and depression (as well as anxiety and substance abuse) before, during, and after the intervention, and followed up 3 and 12 months later.
The investigators found that the BA-TE intervention successfully reduced the symptoms of PTSD and depression both in the traditional in-person delivery as well as in the new telemedicine format. Most important for the main hypothesis of the work, there were no significant differences in effectiveness of the treatment when delivered in person at the clinic or via telemedicine directly to patients' homes. Combining these results with another similar study funded with a VA Merit Review award (#HX00152), the investigators were also able to look for subtle differences in the dropout rate between the two interventions. Using this consolidated data they found that, even though overall dropout rates were 26% in both telemedicine and in-person conditions, participants in the telemedicine group tended to complete more sessions before dropping out. This implies that telemedicine delivered treatment may help increase the total treatment received, even among dropouts (see Figure).
These results suggest that telemedicine delivery of these therapies could be a viable solution to the hurdles of attending in-person sessions at a limited number of clinics. Indeed, a provider at any site could reach a patient anywhere that is convenient or preferable to them. As an added bonus, preliminary cost analysis revealed that the telemedicine delivery was less expensive than in-person therapy. These cost savings would most likely be even more significant in a real world application as the current study did not include service members living in more distant, isolated areas where telemedicine could provide the greatest benefit
Dr. Acierno and his team are now following up on this work through a 2014 DoD Psychological Health Award to test the effectiveness of a telemedicine delivery of therapy for victims of sexual assault. The hope is to find alternatives for those reluctant to attend a crowded treatment facility in-person and ultimately reduce barriers to treatment.
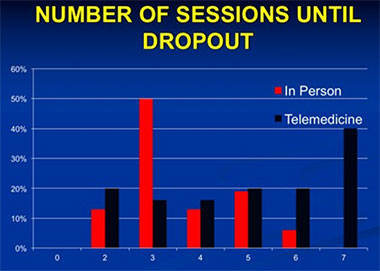
Dropout Rates: Compared to a traditional in-person delivery of PTSD therapy, telemedicine delivery resulted in participants completing more sessions before dropping out of treatment.
Publication:
Acierno, et al. 2016. Behavioral activation and therapeutic exposure for posttraumatic stress disorder: A noninferiority trial of treatment delivered in person versus home-based telehealth. Depress Anxiety. doi: 10.1002/da.22476 [Epub ahead of print]
Links:
Last updated Monday, March 10, 2025














