- SoyCaP: Soy and Prostate Cancer Prevention
- Development of Radioactive Nanocomposites to Treat the Prostate Cancer Microvasculature
- Post-Translational Protein Modification Offers New Molecular Targets Against Prostate Cancer
- Molecular Engineering of Vector-Based Oncolytic and Imaging Approaches for Advanced Prostate Cancer
- Prostaspheres, Enabling the In-depth Characterization of Prostate Stem Cells
- Prostate Cancer Researcher Finds Another Reason to Take Your Vitamins
- Training the Next Generation of HBCU Scientists as Prostate Cancer Researchers
SoyCaP: Soy and Prostate Cancer Prevention
Posted September 23, 2008
Mindy Kurzer, Ph.D., University of Minnesota, Minneapolis, MinnesotaHigh incidence rates of prostate cancer in Western countries versus Asian nations, is often attributed to dietary factors, such as lack of soy consumption. One mechanism by which soy phytoestrogens are thought to be cancer-preventive is via reduction of endogenous sex hormones known to stimulate prostate cell growth. Dr. Mindy Kurzer, a Fiscal Year 2001 New Investigator Awardee, and colleagues Drs. Joel Slaton and Jill Hamilton-Reeves, investigated the effects of soy phytoestrogen consumption on reproductive hormones and prostate tissue markers of cell proliferation and androgen action in men at high risk of prostate cancer. This study was conducted in a cohort of 63 men at high risk of prostate cancer randomized into three groups receiving one of three dietary supplements over a 6-month period: (1) soy protein isolate (SPI+) (107 mg isoflavones/d); (2) alcohol-washed soy protein isolate (SPI-) (< 6 mg isoflavones/d); or (3) milk protein isolate (MPI), each providing 40 g protein/d. Serum hormones (testosterone, dihydrotestosterone, androstenedione, dehydroepiandrosterone, estradiol, estrone, 3a, 17b-androstanediol glucuronide, sex hormone binding globulin), prostate specific antigen, urinary estrogen, and phytoestrogen metabolites were analyzed from urine and blood samples collected from subjects during the study. Similarly, prostate biopsies were performed pre- and post-treatment to evaluate prostate tissue expression of biomarkers for apoptosis (Bax and Bcl-2), proliferation (proliferating cell nuclear antigen [PCNA]), epidermal growth factor receptor (EGFr), estrogen receptor beta (ERb) and androgen receptor (AR) density.
An overall protective effect against prostate cancer was observed in men who received the soy protein regimen. The levels of sex hormone binding globulin (SHBG) and AR protein expression were decreased with the soy protein regimen. Increases in urinary estradiol and estrone concentrations, and an elevation in the 2:16-OH estrone ratio, which has been associated with reduced prostate risk, were also observed. Overall, the effects of the phytoestrogen-free soy powder diet in men were mixed but consistent with a neutral effect on prostate cancer prevention. Given these findings, a larger cohort study (Phase III) examining the protective benefits of soy phytoestrogens in men at high risk of prostate cancer is necessary to determine the efficacy of soy phytoestrogens as a chemopreventive agent.
Publications:
Hamilton-Reeves JM, Rebello SA, Thomas W, Slaton JW, and Kurzer MS. 2008. Effects of soy protein isolate consumption on prostate cancer biomarkers in men at high risk of prostate cancer. Nutrition and Cancer 60 (1):7-13.
Hamilton-Reeves JM, Rebello SA, Thomas W, Slaton JW, and Kurzer MS. 2007. Isoflavone-rich soy protein isolate suppresses androgen receptor expression without altering estrogen receptor beta expression or serum hormonal profiles in men at high risk of prostate cancer. Journal of Nutrition 137:1769-1775.
Hamilton-Reeves JM, Rebello SA, Thomas W, Slaton JW, and Kurzer MS. 2007. Soy protein isolate increases urinary estrogens and the ratio of 2:16?-hydroxyestrone in men at high risk of prostate cancer. Journal of Nutrition 137:2258-2263.
Hamilton-Reeves J and Kurzer MS. 2003. Effects of soy isoflavone consumption on reproductive hormones in males. Soy Connection 11(4):3-5.
Link:
Abstract: Dietary Phytoestrogens and Prostate Cancer Prevention
Development of Radioactive Nanocomposites to Treat the Prostate Cancer Microvasculature
Posted September 23, 2008
Mohamed Khan, M.D., Ph.D., Roswell Park Cancer Institute, Buffalo, New YorkRadiation therapy has been a standard treatment for cancer for many years. However, when cancerous cells are killed with radiation, so are noncancerous cells. Thus, there remains a great need for a more targeted radiation method. Dr. Khan, a Fiscal Year 2002 Idea Development Awardee, is collaborating with Dr. Lajos Balogh at Roswell Park Cancer Institute to develop radioactive composite nanodevices (CNDs) that will access prostate tumors via the leaky tumor microvasculature. CNDs will be retained in the normal microvascular circulature and eventually be excreted. The charge and size selectivity of the CNDs should allow greater disposition of radiation to the cancerous tumor versus normal organs. Toward this goal investigators characterized gold dendrimer CNDs of various sizes, (5, 11, 22, and 53 nm) and different surface charges (negative, positive, or neutral). Analyses of the quantitative biodistribution, excretion, and preliminary toxicity of 11-nm negative surface and 22-nm positive surface CNDs in the B16 mouse melanoma tumor model system were completed. Similarly, 11-nm anionic and 22- and 53-nm cationic CNDs were analyzed in a MatLyLu prostate tumor model for their biodistributions. Although the results of these analyses showed no significant accumulation of the particles in the tumor, the highly quantitative data did emphasize the role of key physiochemical parameters in affecting the biodistribution of nanoparticles. In particular, CNDs of different size and/or surface charge had high levels of selective uptake to specific organs without particular targeting moieties placed on their surfaces. Investigators determined that particle size and charge greatly affected biodistribution of CNDs. These findings have significant implications in the design of all particle-based nanodevices for medical uses and suggest that quantitative physiochemical-based biodistribution studies are important in the design of future "targeted" nanoparticles. This work has been published in several peer-reviewed journals and was recently noted in the January 2008 edition of Nature Nanotechnology under "News and Views of Nanomedicine."
Publications:
Khan MK, Minc LD, Nigavekar S, Kariapper MST, Nair BM, Schipper M, Cook AC, Lesniak WG, Balogh LP. 2008. Fabrication of radioactive gold/dendrimer composite nanodevices and their use for nanobrachytherapy. Nanomedicine: Nanotechnology, Biology, and Medicine 4(1):57-69.
Balogh L, Nigavekar SS, Nair BM, Lesniak W, Zhang C, Sung LY, Kariapper MST, El-Jawahri A, Llanes M, Bolton B, Mamou F, Tan W, Hutson A, Minc L, Khan MK. 2007. Significant effect of size on the in vivo biodistribution of gold composite nanodevices in mouse tumor models. Nanomedicine: Nanotechnology, Biology, and Medicine 3(4):281-296.
Lesniak WG, Kariapper MST, Nair BM, Tan W, Hutson A, Balogh LP, Khan MK. 2007. Synthesis and characterization of PAMAM dendrimer-based multifunctional nanodevices for targeting avb3 integrins. Bioconjugate Chemistry 18(4):1148-1154.
Khan MK, Nigavekar SS, Minc LD, Kariapper MST, Nair BM, Lesniak WG, Balogh LP. 2005. In vivo biodistribution of dendrimers and dendrimer nanocomposites - Implications for cancer imaging and therapy. Technology in Cancer Research and Treatment 4(6):603-613.
Links:
Abstract: Development of Radioactive Nanocomposites to Treat the Prostate Cancer Microvasculature
Abstract: Peptide-Targeted Radioactive Composite Nanodevices Treating Prostate Cancer
Post-Translational Protein Modification Offers New Molecular Targets Against Prostate Cancer
Posted September 23, 2008
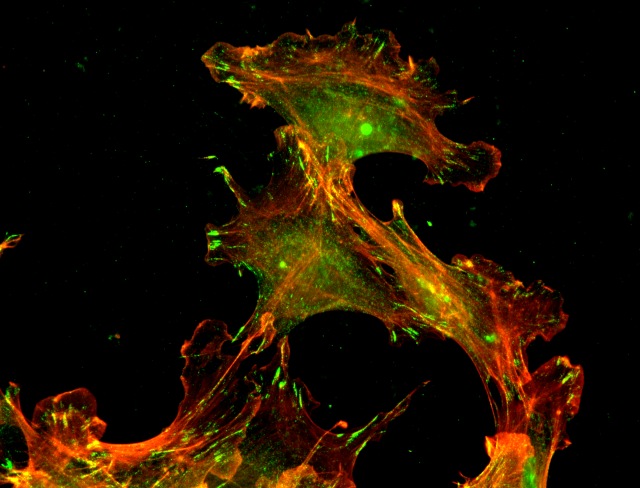
Anna S. Kashina, Ph.D., University of Pennsylvania, Philadelphia, PennsylvaniaPost-translational modification is a biochemical event that regulates enzymes that control various cellular growth signals. Fiscal Year 2004 New Investigator Awardee Dr. Anna Kashina and colleagues are investigating the relationship between protein arginylation (post-translational modification process) and prostate cancer progression and metastasis. The transfer of arginine residues from transfer-RNA (t-RNA) onto the N-terminus of proteins occurs via arginyl-tRNA-protein transferase (ATE1) enzyme, resulting in a stable peptide bond. ATE1 knockout mice show defects in cardiovascular development and angiogenesis. Dr. Kashina's research has demonstrated that arginylation regulates cell structure, intracellular assembly, and motility by modifying a single protein target, beta-actin, a key component of the cytoskeleton and the cell leading edge. Although this post-translational addition of arginyl groups to proteins is known to be critical for the embryonic development and survival of an organism, the identity of the arginylated proteins and the global effects of arginylation in vivo are largely unknown. Dr. Kashina and colleagues successfully developed a technique that utilizes ATE1 knockout mice, two-dimensional gel electrophoresis, metabolic labeling of arginine, immunoaffinity chromatography, and mass spectrometry to identify key arginylated proteins in vivo to gain insights into complex biological functions of this modification. The results of the study reveal that arginylation is a global regulatory mechanism for controlling vital physiological processes. These findings offer potentially new tools and approaches to prostate cancer therapy.
Absence of arginylation induces changes in cell motility and promotes invasive behavior characteristic for cancer cells. Co-staining of an invading cell monolayer in culture with actin cytoskeleton (red) and cell attachment (green) markers.
Publications:
Wong CCL, Xu T, Rai R, Bailey AO, Yates III JR, Wolf YI, Zebrosky H, and Kashina A. 2007. Global analysis of posttranslational protein arginylation. PLoS Biology 5(10):1-12.
Karakozova M, Kozak M, Wong CCL, Bailey AO, Yates III JR, Mogilner A, Zebroski H, and Kashina A. 2006. Arginylation of beta-actin cytoskeleton and cell motility. Science 313:192-196.
Link:
Molecular Engineering of Vector-Based Oncolytic and Imaging Approaches for Advanced Prostate Cancer
Posted September 17, 2008
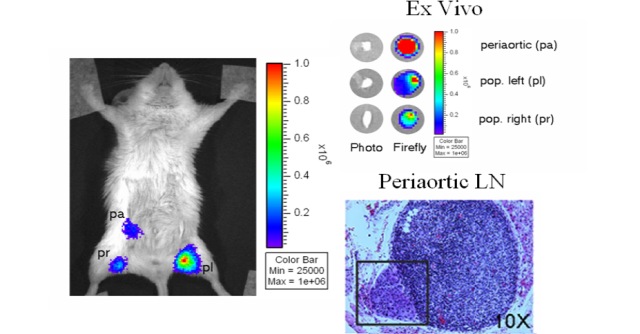
Lily Wu, M.D., Ph.D., University of California, Los AngelesThe presence of pelvic lymph node metastases in prostate cancer patients is a predictor of poor outcome and is crucial to diagnosing disease status and identifying appropriate treatment options. The assessment of lymph node disease is currently determined by pelvic lymphadenectomy. Unfortunately, the procedure results in approximately 20% of prostate cancer patients developing adverse complications including venous thrombosis and pulmonary embolism. Thus, a noninvasive diagnostic tool for the detection of sentinel lymph node metastases is needed. A Fiscal Year 2002 Idea Development Award to Dr. Lily Wu, of UCLA, seeded the development of recombinant human prostate-specific adenoviruses equipped to express optical and positron emission tomography (PET) imaging reporter genes under the transcriptional control of a prostate-specific enhancer element to detect metastatic prostate cancer cells. In a recent advancement, Dr. Wu exploited the innate lymphotropic properties of adenovirus particles injected into the prostate near a tumor mass, leading the particles to the draining or sentinel lymph nodes that harbored metastases of human prostate cancer in a mouse xenograft model. Using optical and PET imaging technology, Dr. Wu has shown that the reporter gene is delivered to and expressed in prostate cancer metastases in the draining lymph nodes, which enables the visualization of both large macroscopic and occult nodal lesions in the living animals. The PET approach for imaging gene expression reported by Dr. Wu in this study is directly applicable to patients. The prospect of coupling this detection methodology with suicide-gene therapy is of the utmost clinical relevance, especially to African American men with metastatic prostate cancer, where the 5-year survival rate is approximately 30%.
Publications:
Burton JB, Johnson M, Sato M, Koh SB, Stout D, Mulholland D, Chatziioannou AF, Phelps M, Wu H, Wu L. 2008. Adenovirus mediated gene expression imaging to directly detect sentinel lymph node metastasis of prostate cancer. Nature Medicine 8:882-888.
Sato M, Figueiredo ML, Burton JB, Johnson M, Chen M, Powell R, Gambhir SS, Carey M, Wu L. 2008. Configurations of a two-tiered amplified gene expression system in adenoviral vectors designed to improve the specificity of in vivo prostate cancer imaging. Gene Therapy 8:583-593.
Brakenhielm E, Burton JB, Johnson M, Chavarria N, Morizono K, Chen I, Alitalo K, Wu L. 2007. Modulating metastasis by a lymphangiogenic switch in prostate cancer. International Journal of Canada 121:2153-2161.
Johnson M, Sato M, Burton J, Gambhir SS, Carey M, Wu L. 2005. MicroPET/CT monitoring of herpes thymidine kinase suicide gene therapy in a prostate cancer xenograft: The advantage of a cell-specific transcriptional targeting approach. Molecular Imaging 4:463-472.
Sato M, Johnson M, Zhang L, Gambhir SS, Carey M, Wu L. 2005. Functionality of androgen receptor-based gene expression imaging in hormone refractory prostate cancer. Clinical Cancer Research 11:3743-3749.
Links:
Prostaspheres, Enabling the In-depth Characterization of Prostate Stem Cells
Posted June 30, 2008
Isla Garraway, M.D., Ph.D., University of California, Los Angeles, CaliforniaRecent studies in multiple organ systems have focused on cancer stem cells (CSCs), which represent a small minority of cells within tumors but are suspected to be largely responsible for cancer propagation. Developing drugs that target CSCs may result in better clinical outcomes. As a first step toward this goal, Dr. Isla Garraway, a Fiscal Year 2006 (FY06) Exploration - Hypothesis Development Awardee, and colleagues have begun development of an assay that allows the cultivation of rare CSCs in solid tumors. The assay utilizes prostapheres, globes of stem and early progenitor cells derived from human tissue specimens, which can be induced to grow in culture. Prostate tissue specimens from 60 patients undergoing cancer surgery were collected for the isolation and characterization of the prostaspheres. Their biomarker expression pattern was found to most closely resemble normal basal cells, with predominately CK5, CD44, alpha integrin (CD49f), and p63 expression. Subcutaneous injection of the prostaspheres into immunocompromised mice resulted in xenograft formation of structures resembling partially differentiated prostate glands. These glands demonstrated expression of several prostate markers, including prostate stem cell antigen, androgen receptor, CK5, CK8, and p63. The prostasphere assay may enable enrichment of stem cells from normal and cancerous specimens for further characterization, enabling the identification of new therapeutic targets.
Dr. Garraway is also the recipient of two additional awards from the Department of Defense. A FY05 New Investigator Award was used to develop a new transgenic mouse model, TRAMP-TVA, which allows disease progression to be followed and therapeutic interventions to be imaged. Additionally, efficient transfer of small hairpin ribonucleic acid molecules into epithelial cells will allow specific genes that are thought to be important in prostate cancer invasion and metastases to be studied. More recently, Dr. Garraway received a FY07 Physician Research Training Award to further develop conditions under which prostaspheres harboring the TMPRSS2:ERG fusion form and understand the unique properties of these prostate cancer stem cells. These studies will enhance the identification and characterization of prostate cancer stem cells and better distinguish the fundamental differences between these cells and normal prostate stem cells in extended culture and exposure to androgen. Results from these studies on prostaspheres from prostate tumor and normal tissues could lead to new therapeutic treatment strategies to block progression of prostate cancer.
Links:
Abstract: Development of a Mouse Model for Prostate Cancer Imaging and Study of Disease Progression
Prostate Cancer Researcher Finds Another Reason to Take Your Vitamins
Posted March 6, 2008
Yi-Fen Lee, Ph.D., University of Rochester, Rochester, New YorkThe importance of vitamin D in maintaining bone health and normal calcium metabolism is well-known, but recent evidence suggests that vitamin D may also be a powerful addition to the arsenal for cancer prevention and treatment. Dr. Yi-Fen Lee, an Associate Professor at the University of Rochester and recipient of a Department of Defense Fiscal Year 2004 Prostate Cancer Research Program (PCRP) New Investigator Award, is investigating calcitriol (1a,25-dihydroxyvitamin D3), the active form of vitamin D that potently inhibits tumor cell growth and angiogenesis. Dr. Lee found that calcitriol impaired prostate cancer-induced neovascularization by blocking expression of the secreted angiogenic factor interleukin-8, which was upregulated in human prostate cancer and pre-malignant prostate tissue relative to benign tissue. She also explored the potential utility of calcitriol for the treatment of advanced prostate cancer, for which there are few therapeutic options. Calcitriol was shown to enhance the growth inhibitory effects of docetaxel, a drug commonly used for treating hormone-refractory prostate cancer. The actions of calcitriol were mediated by increased expression of the pro-apoptotic protein Bax and reduced expression of multidrug resistance-associated protein-1. Dr. Lee's studies demonstrate the potential for calcitriol as a chemopreventive therapy as well as a chemosensitizing agent for the treatment of advanced prostate cancer. Moreover, her successes illustrate the potential of the PCRP New Investigator Award to foster early-career prostate cancer researchers. This award has assisted Dr. Lee in further developing her research program in nuclear receptors, aging, and prostate cancer, for which she also has an active grant from the American Cancer Society.
Publications:
Bao BY, Yao J, Lee YF. 2006. 1alpha, 25-dihydroxyvitamin D3 suppresses interleukin-8-mediated prostate cancer cell angiogenesis. Carcinogenesis 27(9):1883-93 [Epub 2006 Apr 19].
Ting HJ, Hsu J, Bao BY, et al. 2007. Docetaxel-induced growth inhibition and apoptosis in androgen independent prostate cancer cells are enhanced by 1alpha,25-dihydroxyvitamin D3. Cancer Letters 8:247(1):122-9 [Epub 2006 Apr 27].
Link:
Training the Next Generation of HBCU Scientists as Prostate Cancer Researchers
Posted February 11, 2008
Jamboor K. Vishwanatha, Ph.D., University of North Texas Health Science Center, Fort Worth, TexasThe Prostate Cancer Research Program (PCRP) Collaborative Undergraduate Historically Black Colleges and Universities (HBCU) Student Summer Training Program Award (STPA) was created to encourage HBCU students to pursue careers in prostate cancer research. In addition, this training will enable the students to serve both as sources of education on prostate cancer treatment and as advocates of cancer screening in their communities. Since the creation of this award mechanism in Fiscal Year 2004, 11 STP awards have been granted to nine laboratories with expertise in prostate cancer research. Thus far, more than 60 HBCU students have received hands-on comprehensive mentored training and education.
One such successful program is being conducted by Dr. Jamboor K. Vishwanatha at the University of North Texas Health Science Center. Five students recently participated in this 10-week summer program in 2007. Students were chosen by means of a highly competitive selection process and had an opportunity to work in the laboratory with a prostate cancer scientist. The students also attended weekly seminars, which included sessions on stem cells, cancer, and forensic genetics, and participated in a learning and study skills workshop. The students were also provided with a GRE preparation course and a course in health disparities. At the end of the summer, each student prepared an abstract of his or her work and presented it at a student research symposium.
This award program has seen much success, despite having only been in existence since 2004. A majority of the STPA participants have been accepted by or are planning to enroll in Ph.D. or M.D. programs. Students have been so inspired by their summer training experiences that many have expressed to their mentors their commitment to pursue studies in prostate cancer research.
Link: