Prostate Cancer
CDK12 loss is a distinct immunogenic class of advanced prostate cancer



Posted September 25, 2018
Marcin Cieslik, Ph.D., University of Michigan

University of Michigan
Prostate cancer is a heterogeneous disease, meaning that not all prostate cancer cells will progress at the same rate, and they may vary in their response to different therapies which will ultimately affect a patient's overall survival. This heterogeneity stems from differences that exist the molecular level, so researchers have been looking to identify prognostic biomarkers to guide treatment decisions. Dr. Marcin Cieslik and his colleagues at the University of Michigan hypothesized that cellular immune signatures, such as tumor infiltrating lymphocytes (TILs) and immune checkpoints, can predict survival in metastatic castration-resistant prostate cancer (mCRPC). Furthermore, this difference in survival could be due to a stronger and more diverse immune phenotype that could result in better outcomes to immunotherapy, which has been an elusive treatment strategy for prostate cancer patients in general.
Dr. Cieslik's team began by focusing their research on a specific subtype of prostate cancer cells that contain mutations in the CDK12 gene. CDK12 is a cyclin-dependent kinase that regulates several critical cellular processes, and previous work from this group has shown that CDK12 mutations are enriched in mCRPC. With support from a FY16 Idea Development Award, Dr. Cieslik examined the ability of immune cells to infiltrate and escape from CDK12-mutant mCRPC tumors, and the results confirmed that CDK12-mutant prostate cancer is a unique molecular subtype associated with extensive immune infiltration. Specifically, CDK12-mutant tumors showed an increased expression of immune signaling proteins, called chemokines, and their receptors, which presumably allowed for better infiltration of the immune cells into the mCRPC tumors. This data suggest that patients whose mCRPC contains CDK12 mutations may respond well to immunotherapy, justifying further investigation at the clinical level.
These results are now being translated to patients through an investigator-initiated Phase II clinical trial titled "Immunotherapy in Patients with Metastatic Cancers and CDK12 Mutations (IMPACT)." This multi-center trial is being sponsored by University of Michigan Cancer Center with Dr. Ajjai Alva as the principal investigator, and will also be recruiting patients at the Memorial Sloan Kettering Cancer Center and the University of California San Francisco. This Phase II study will evaluate the efficacy of checkpoint inhibitor immunotherapy (nivolumab and ipilimumab combination therapy followed by nivolumab monotherapy) in mCRPC patients with CDK12 mutant tumors, and is now open for enrollment (see NCT03570619 on clinicaltrials.gov for more information). Further validation of Dr. Cieslik's hypothesis in the clinic would not only benefit the practice of precision medicine for men with mCRPC, but may also provide answers for how to better harness the power of immunotherapy for other disease subtypes.
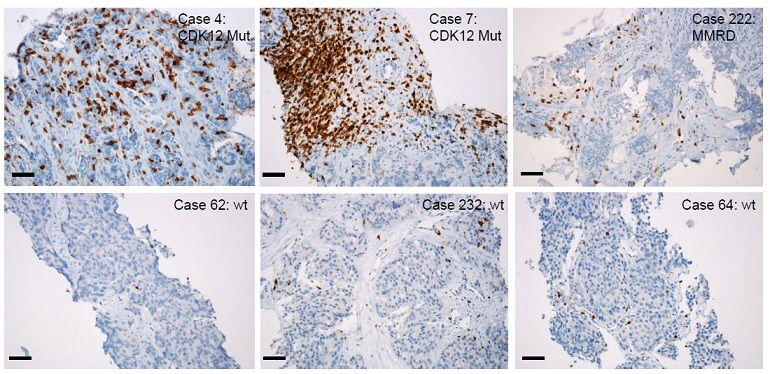
Publication:
Wu, Y.-M., Cieslik, M. , Lonigro, R.J., et al. 2018. Inactivation of CDK12 Delineates a Distinct Immunogenic Class of Advanced Prostate Cancer. Cell 173, 1770:1782.e14.
Link:
Regulatory Networks of Immune Evasion in Metastatic Prostate Cancer
Last updated Monday, March 10, 2025














