Prostate Cancer
Statin use may increase survival in men with prostate cancer undergoing androgen deprivation therapy



Posted December 22, 2017
Philip Kantoff, M.D., Memorial Sloan Kettering Cancer Center

One of the mechanisms of resistance to androgen deprivation therapy (ADT) for prostate cancer (PCa) is persistent androgen receptor signaling. Part of the reason for this is persistent production of testosterone even in the castrated state. Conversion of androgen precursors to testosterone inside the PCa cell appears to be an important mechanism. The import of androgens into cells can efficiently occur through members of the super family of organic anion transporting polypeptides (OATPs) encoded by SLCO (Solute Carrier Organ Anion Transporter Family) genes, which mediate the sodium-independent uptake of a wide variety of endogenous compounds and drugs into cells.
Dr. Philip Kantoff initiated these studies with colleagues while at the Dana-Farber Cancer Institute and showed that SLCO2B1 mediates efficient uptake of the important androgen precursor, DHEAS, in cell lines. Additionally, they have demonstrated that certain SLCO2B1 inherited genetic variants, which allow greater expression and/or more efficient import of androgen, enhance cell growth and are associated with a shorter time to progression on ADT and decreased survival. Further, SLCO2B1 is expressed at a higher level in advanced PCa tumors than localized PCa.
Statins, which are widely used in the United States because of their lipid lowering properties, have also been shown in some cohort and case control studies to decrease recurrence and mortality from PCa, although the precise mechanism of how PCa patients benefit from statin use is largely unknown. Since it is established that statins utilize SLCO2B1 to enter cells, Dr. Kantoff and his research team hypothesized that the drug may compete with DHEAS uptake and that statin use might prolong time to progression while on ADT. With funding from a FY13 Idea Development Award, they used preclinical models to show that statins competitively interfered with the uptake of DHEAS into cells and that this process was mediated by the transporter SLCO2B1. Additionally, they showed that in a large cohort study of men being treated with ADT, men who were taking statins had a longer time in remission on ADT. To further validate these findings, they further looked at the impact of statin use on response duration to the second generation androgen synthesis inhibitor, abiraterone acetate. Similarly, they found a trend toward longer duration of response, although this did not reach statistical significance.
These findings demonstrate that statin use may be beneficial to improve outcomes for men with PCa undergoing ADT. Furthermore, Dr. Kantoff's work shows that statins and DHEAS compete for the same transporter, SLCO2B1, and that administration of statins competitively reduces uptake of DHEAS and tumor cell growth. These results provide a plausible mechanism to support their clinical observations. Dr. Kantoff is now the Chairman of the Department of Medicine at Memorial Sloan Kettering Cancer Institute where he continues his studies to help further characterize the role of statins as anticancer therapies for PCa patients.
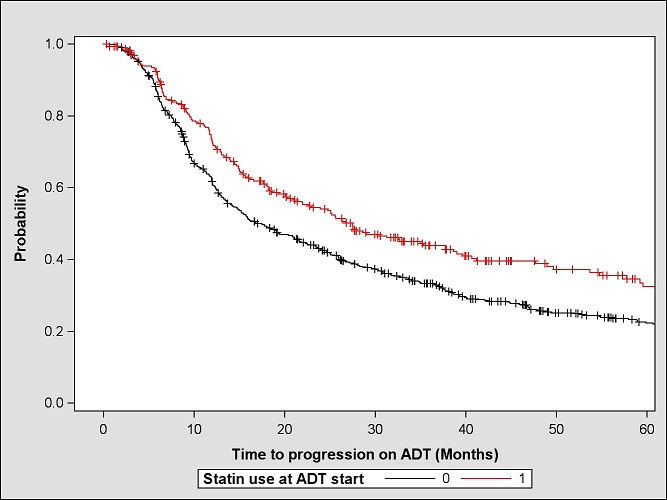
Impact of statin use on the time to progression prostate cancer patients undergoing androgen deprivation therapy
Publications:
Harshman L, Werner L, Tripathi, A et al. 2017. The impact of statin use on the efficacy of abiraterone acetate in patients with castration-resistant prostate cancer. The Prostate 77, 1303-1311
Wang X, Harshman LC, Xie W, et al. 2016. Association of SLCO2B1 genotypes with time to progression and overall survival in patients receiving androgen deprivation therapy for prostate cancer. J Clin Oncol 34(4):352-359.
Harshman LC, Wang X, Nakabayashi M, et al. 2015. Statin use at the time of initiation of androgen deprivation therapy and time to progression in patients with hormone-sensitive prostate cancer. JAMA Oncol 1:495-504.
Link:
SLCO2B1 and SLCO1B3 as New Targets for Enhancing Androgen Deprivation Therapy for Prostate Cancer
Last updated Friday, December 13, 2024














