


Posted February 13, 2014
Dr. Mohammad Saleem (Bhat), Ph.D., The Hormel Institute, University of Minnesota
 Castration-resistant prostate cancer (CRPC) is a hard-to-treat disease, and little is known about the reasons contributing to this form of prostate cancer. Thus, identification of one or more critical molecules involved in conferring chemoresistance would be an important advancement in developing new ways to prevent or treat this deadly form of the disease. Recent advancements in cancer genomics have paved a way to understanding the causes/mechanisms underlying chemoresistance and survival of prostate tumor cells during and after chemotherapy. Recent reports indicate involvement of several genes, one such group being the Polycomb gene repressor family, which has been associated with several types of cancer including prostate cancer. The emergence of a specific member of the polycomb family, BMI1, as a gene with involvement in cancer stem-cell renewal makes it an attractive target for further investigation.
Castration-resistant prostate cancer (CRPC) is a hard-to-treat disease, and little is known about the reasons contributing to this form of prostate cancer. Thus, identification of one or more critical molecules involved in conferring chemoresistance would be an important advancement in developing new ways to prevent or treat this deadly form of the disease. Recent advancements in cancer genomics have paved a way to understanding the causes/mechanisms underlying chemoresistance and survival of prostate tumor cells during and after chemotherapy. Recent reports indicate involvement of several genes, one such group being the Polycomb gene repressor family, which has been associated with several types of cancer including prostate cancer. The emergence of a specific member of the polycomb family, BMI1, as a gene with involvement in cancer stem-cell renewal makes it an attractive target for further investigation.
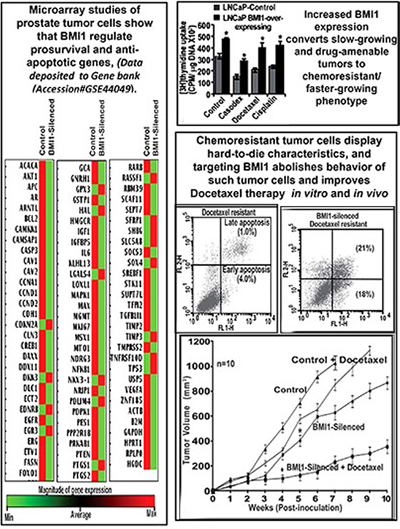
Dr. Mohammed Saleem, (Bhat), recipient of a New Investigator Award from the DoD Prostate Cancer Research Program, along with his research team at The Hormel Institute, University of Minnesota, has provided compelling evidence that BMI1 plays a crucial role in determining the fate of tumors treated with chemotherapy. By employing a number of assays such as microarray, ChIP, immunoblot and Luciferase reporter assays, they identified a unique mechanism through which BMI1 rescues tumor cells from chemotherapy by regulating the activity and binding of the TCF4 transcription factor to the control region of BCL2, an anti-apoptotic gene. They also noticed that BMI1 is capable of driving normal cells to an over-active growth state by breaking their normal process of aging and death (senescence), suggesting that BMI1 might be play a critical role in breaking the sleeping mode of tumor cells and driving them towards proliferation. The fact that BMI1 expression is not influenced by androgen, which is the target of most chemotherapy treatments, further suggests that BMI1 might play a role in driving indolent disease to a more aggressive, androgen-independent disease state.
Dr. Saleem's group also tested the ability of BMI1 blockade to enhance the results of docetaxel treatment, a commonly used therapy that can lower PSA levels by more than 50% but is not able to completely eliminate the tumor. Using a mouse xenograft model, they showed that targeting BMI1 in chemoresistant cells sensitizes them to docetaxel therapy, and that the success of docetaxel therapy in the xenograft mouse model was highly dependent on the level of BMI1. This suggests that (i) targeting BMI1 should be a part of therapeutic strategy to combat chemoresistant cancer, and (ii) BMI1-specific interventions may provide opportunities to enhance the efficacy of chemotherapy in a large group of prostate cancer patients.
Publications:
Links:














