Posted September 3, 2013
Michael Ittmann, M.D., Ph.D., Baylor College of Medicine
Bulent Ozpolat, M.D., Ph.D., M.D. Anderson Cancer Center
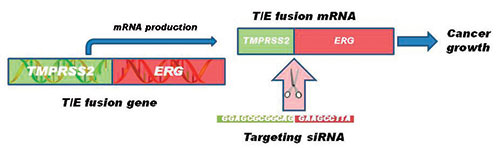
 The TMPRSS2/ERG (T/E) fusion gene occurs in 50% of prostate cancers and is believed to promote tumor growth and invasion, making it an outstanding therapeutic target. The T/E mRNA fusion junctions (where the two genes come together) are present only in prostate cancer cells, and it is believed that developing gene silencers (siRNAs) highly specific for this sequence could target prostate cancer without off-target effects in normal tissues, minimizing toxicity.
The TMPRSS2/ERG (T/E) fusion gene occurs in 50% of prostate cancers and is believed to promote tumor growth and invasion, making it an outstanding therapeutic target. The T/E mRNA fusion junctions (where the two genes come together) are present only in prostate cancer cells, and it is believed that developing gene silencers (siRNAs) highly specific for this sequence could target prostate cancer without off-target effects in normal tissues, minimizing toxicity.
Dr. Michael Ittmann and his research team at Baylor College of Medicine began working on the T/E fusion gene 6 years ago, and have shown that knocking down T/E expression inhibits tumor growth in engineered cells growing in mice. They realized that they could target the junction of the T/E gene to make the gene knockdown highly specific. Dr. Bulent Ozpolat and his research team at M. D. Anderson Cancer Center were also concurrently developing nanoliposomal vectors for delivering siRNAs (small interfering RNA molecules) to tumors. Thus, with support from a FY08 Synergistic Idea Development Award, Dr. Ittmann and Dr. Ozpolat combined their areas of expertise to successfully develop an optimal T/E fusion siRNA, which was able to knock down expression of the T/E fusion gene and suppress tumor growth without any apparent toxicity.
Tumor growth inhibition by nanoliposome siRNAs was somewhat variable, and correlated with the degree of T/E fusion gene knockdown. In addition, silencing the T/E fusion gene makes prostate cancer cells more sensitive to chemotherapy and radiation, so the research teams are exploring the potential for nanoliposomal gene knockdown therapy as a low toxicity means of enhancing the effectiveness of these common therapies. As nanoliposomes are currently moving toward clinical trials in other cancers, Drs. Ittmann and Ozpolat are seeking to optimize this novel nanoliposome approach for translation into clinical testing in patients and ultimately improve prostate cancer treatment.