


Posted June 7, 2016
Caterina Mainero, M.D., Ph.D., Massachusetts General Hospital
 Multiple sclerosis (MS) is an immune-mediated chronic disease of the central nervous system, pathologically characterized by inflammation, demyelination, and neurodegeneration. Post-mortem studies from late-stage MS patients suggest that cortical demyelinating lesions (lesions on the cortex/outer surface of the cerebrum) are an important correlate of disease progression. Further evidence suggests that these lesions are driven by neuroinflammation on the cortex, independent from other areas of the brain.
Multiple sclerosis (MS) is an immune-mediated chronic disease of the central nervous system, pathologically characterized by inflammation, demyelination, and neurodegeneration. Post-mortem studies from late-stage MS patients suggest that cortical demyelinating lesions (lesions on the cortex/outer surface of the cerebrum) are an important correlate of disease progression. Further evidence suggests that these lesions are driven by neuroinflammation on the cortex, independent from other areas of the brain.
Dr. Mainero received a fiscal year 2012 (FY12) MSRP Idea Award to evaluate inflammation and structural tissue changes in the cortex of patients with MS and to test her hypothesis that there is a correlation between cortical inflammation and cortical demyelination. To assess cortical characteristics and characterize any observed abnormalities, Dr. Mainero developed an advanced MRI method (7 Tesla, T, MRI) that has demonstrated greater sensitivity in identifying cortical lesions than conventional MRI techniques. The observed neuroinflammation in MS is thought to be caused by activated microglia, which are ubiquitous immune cells found in the brain. Activated microglia upregulate expression of a specific translocator protein called TSPO on the cellular surface. Using a labeled TSPO ligand called [¹¹C]-PBR28, positron emission tomography (PET) methods can be used to quantify the activated microglia in the brains of MS patients.
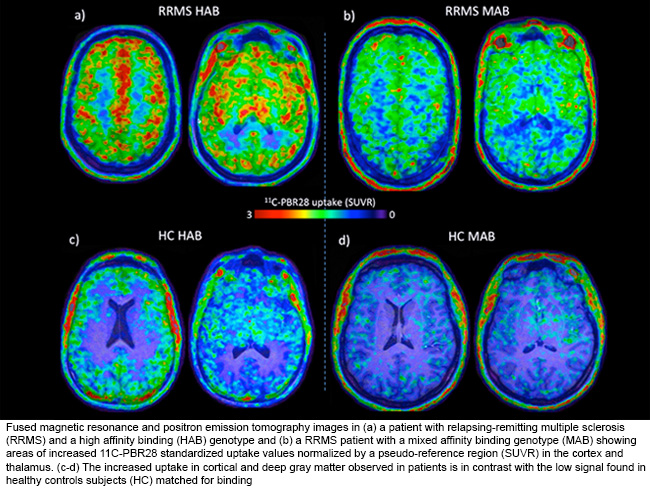
The combination of these two techniques has allowed Dr. Mainero to demonstrate in vivo the presence of diffuse microglia activation in the brains of MS patients. However, inflammation was most prominent in both cortical lesions and subcortical gray matter (i.e., the thalamus, hippocampus, and basal ganglia). The use of ultra-high resolution information from 7T MRI scans was crucial for identifying focal cortical lesions, which were otherwise not visible on lower resolution MRI images. This is the first time that a specific increase in TSPO binding is reported for cortical lesions in MS in vivo.
In addition, Dr. Mainero was able to show that high-resolution [¹¹C]-PBR28 PET imaging can detect in vivo diffuse inflammation in different brain tissue compartments in MS. But this observation is most prominent in the cortex, cortical lesions, and deep gray matter. Dr. Mainero was able to determine that the degree of inflammation in the cortex and deep gray matter is associated with neurological disability, impaired information processing speed, and neurodegeneration. Additionally, microglia activation, especially in the cortex, thalamus, and normal-appearing white matter, was associated with neurodegeneration and negatively impacted physical disability and cognitive performance (information processing speed) in MS patients.
High-resolution [¹¹C]-PBR28 MR-PET imaging is positioned to be a promising tool for assessing in vivo microglia activation within different brain tissue compartments in MS patients, particularly in the cortex, cortical lesions, and subcortical gray matter.
Publication:
Mainero C, Louapre C, Govindarajan ST, Gianní C, Nielsen AS, Cohen-Adad J, Sloane J, Kinkel RP. 2015. A gradient in cortical pathology in multiple sclerosis by in vivo quantitative 7 Tesla imaging. Brain 138(Pt 4):932-945. PMID: 25681411.
Louapre C, Govindarajan ST, Gianní C, Langkammer C, Sloane JA, Kinkel RP, Mainero C. 2015. Beyond focal cortical lesions in MS: an in vivo quantitative and spatial imaging study at 7 T. Neurology 85(19):1702-1709. PMID: 26468411.
Herranz E, Gianní C, Louapre C, Treaba CA, Govindarajan ST, Mangeat G, Ouellette R, Loggia M, Ward N, Klawiter EC, Sloane JA, Catana C, Hooker JM, Kinkel RP, Mainero C. 2016. The neuroinflammatory component of gray matter pathology in multiple sclerosis by in vivo combined 11C-PBR28 MR-PET and 7T imaging. #4606. Proceedings of the 24th Meeting of the International Society for Magnetic Resonance in Medicine (ISMRM), Singapore.
Link:














