Lung Cancer



Posted November 18, 2022
Christopher Vakoc, Ph.D., Cold Spring Harbor Laboratory

Dr. Christopher Vakoc
(Photo provided)
Small cell lung cancer (SCLC) comprises an aggressive subset of total lung cancer cases that typically present as late-stage and widespread disease with poor prognosis. Though historically treated as a single disease, recent studies have demonstrated that several lineage variants of SCLC exist, which have the potential to predict different sensitivities to novel cancer drugs. Therefore, understanding the unique molecular drivers for each variant of SCLC is critical in the development of more tailored therapeutics. With assistance from a Fiscal Year 2018 Lung Cancer Research Program Idea Development Award (Established Investigator), Dr. Christopher Vakoc has been investigating one variant of SCLC tumors that arise from tuft cells (SCLC-P) to uncover their Achilles' heel. Striking early findings have revealed that two previously undescribed proteins, OCA-T1 or OCA-T2, can form a complex with a transcription factor called POU2F3 within tuft cells. These cells are critical for tuft cell identity as well as SCLC-P development. This discovery provides both novel insight into SCLC-P and a unique molecular vulnerability for therapeutic development.
Tuft cells are found in the mucosal lining of the airways and other organ systems and normally function as sentinels to mediate local immune response to foreign pathogens. Interestingly, the tuft cell variant of SCLC was only recently characterized and is marked by the obligate expression of the POU2F3 transcription factor. As reported in Nature, Dr. Vakoc's team profiled tuft cells from mouse and human tissues and found that an undescribed gene, OCA-T1, was expressed in these cells in a pattern that resembles POU2F3. Further, the group found that OCA-T1 was uniquely expressed in SCLC-P cancer cell lines and no other cancer type or SCLC variant. This observation led the group to perform a search for other potential gene products that resembled OCA-T1, which resulted in the discovery of a second unstudied gene, OCA-T2, that was found to be expressed in tuft cells; however, OCA-T2 was expressed at lower levels than OCA-T1 and could be detected in a subset of SCLC-P cancer cell lines that do not express OCA-T1, an important distinction.
The research team next performed experiments designed to determine the importance of OCA-T1 or OCA-T2 in tuft cell and SCLC-P biology. They found that both proteins would form a stable complex with POU2F3 in the presence of DNA and that these complexes are found at unique and overlapping DNA binding sites within the genome. Further, the removal of either OCA-T1, OCA-T2, or POU2F3 from SCLC-P cells caused a highly similar change in the genes expressed by the cells. In addition, tuft cell-specific genes could be activated by forcing the expression of POU2F3 and OCA-T1 (or OCA-T2) in non-tuft cell culture models, but only when both POU2F3 and OCA-T1 (or OCA-T2) were present and not individually. These findings suggest that OCA-T1 or OCA-T2 act as co-activators of gene expression with POU2F3 in tuft cells and in SCLC-P.
Dr. Vakoc's group also examined the effects of removing POU2F3, OCA-T1, or OCA-T2 on SCLC-P pathology and found that inactivation of any of the three genes within SCLC-P cells rendered them unable to proliferate or form measurable tumors in mice. The team also determined that these effects were due to the specific binding of OCA-T1 (or OCA-T2) to POU2F3. Further, knockout of OCA-T1 from the developing mouse caused the near-complete loss of tuft cells throughout the animal, though no other obvious physiological defects were observed.
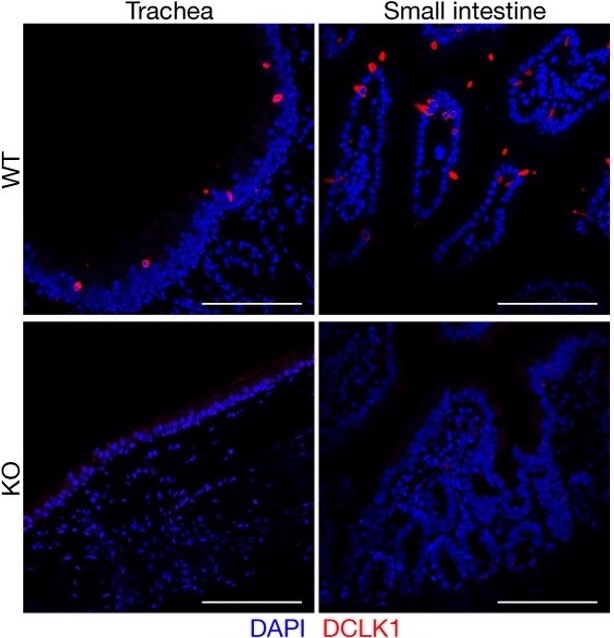 Figure 1: OCA-T1 knockout (KO) mice are devoid of tuft cells (labeled in red with a tuft cell marker DCLK1), which are present in normal wild-type (WT) mice.1 (Figure provided by Dr. Christopher Vakoc)
Figure 1: OCA-T1 knockout (KO) mice are devoid of tuft cells (labeled in red with a tuft cell marker DCLK1), which are present in normal wild-type (WT) mice.1 (Figure provided by Dr. Christopher Vakoc)
Combined, the efforts of Dr. Vakoc and his research team so far point to a specific and critical role for the newly discovered OCA-T1 and OCA-T2 genes in both normal and malignant tuft cell biology. This deeper understanding of the SCLC-P variant holds the promise of a novel molecular interaction that could be specifically disrupted by small molecule interventions and only within the cells of concern. This is the very definition of the patient-specific and tailored therapeutic approaches that will be required as we seek the next generation of lung cancer interventions.
Publications:
1Wu XS, He X-Y, Huang Y-H, et al. 2022. OCA-T1 and OCA-T2 are coactivators of POU2F3 in the tuft cell lineage. Nature. 607, 169-175.
Last updated Wednesday, September 17, 2025
 An official website of the United States government
An official website of the United States government
 ) or https:// means you've safely connected to the .mil website. Share sensitive information only on official, secure websites.
) or https:// means you've safely connected to the .mil website. Share sensitive information only on official, secure websites.
