Consumer Involvement



The views, opinions, and/or findings contained in this paper are those of the author(s) and should not be construed as an official Department of Defense position, policy or decision
Posted July 20, 2022
 Annie Horner (Photo Provided)
Annie Horner (Photo Provided)
My cancer story began in the spring of 2016 when I was 18 years old. I was taking college classes at Georgia State and volunteering at Children's Healthcare of Atlanta through the College Volunteer program, as I had an interest in pursuing a career in a hospital setting working with children. One day, my mom noticed a pea sized bump near my left wrist. It didn't hurt and it was so small that if I moved my hand a certain way, it would recede and disappear into my arm. We thought it was a little strange, but we weren't particularly worried. Ten days later I was shocked to see that I had a very large bump in this same location. The pea had grown, seemingly overnight, into the size of a lemon.
I had not recalled bumping or injuring my arm, so I went immediately to the doctor to get it checked out. Unfortunately because of my age, I had just recently transitioned from the care of my lifelong pediatrician to a new adult primary care doctor. This was an unfamiliar setting in which to navigate, and I felt like a nameless, faceless patient. It would take several weeks to get a diagnosis. My new primary care doctor examined my bump, said that it was not a lipoma (which I had never heard of) because it grew so rapidly, and wrote a script for an x-ray, which I got that same day. The x-ray showed that the bone was normal but there was swelling of the soft tissues, which the doctor said would resolve on its own. Although this sounded like good news, I knew I hadn't injured my arm, so it didn't make sense to me that it was just swelling that would heal. Two days later I reached out to another doctor who ordered an ultrasound. The ultrasound showed a mass that was not fluid filled and so was not a cyst. I didn't understand the significance of this not being fluid filled but the doctor was not concerned and said he would check it in a follow up appointment in several weeks. A day or two before the appointment, my hand started going numb and I felt little electrocution-like shocks. At my appointment, this doctor took one look at my forearm and I knew by the look on his face that he was worried. He told me that he was going to call an orthopedic oncologist (a type of doctor I had never heard of) for an opinion and that in the meantime he was sending up prayers. I went into some sort of weird state, where I became scared but was also in denial, thinking that surely the worst-case scenario was that I might need a surgery to remove it so that it wouldn't keep growing and cause more numbness, but that it surely wouldn't be cancer or anything! Things happened very quickly after that. I met right away with the orthopedic oncologist, who ordered an immediate MRI...this led to biopsies of the mass the very next day. The orthopedic oncologist noted that the tissue did not look like healthy tissue. He put on his white coat, picked up the tray with pieces of tissue, and kindly and gently told me that he would personally take the samples to the pathologist, remain at his side during examination, and return to me with a preliminary diagnosis in about an hour. I was feeling sick with fear but at the same time told myself that this would be over soon and I would have good news. However, when the doctor returned, he told me very gently that it was a malignancy. The doctor went on to explain that I had a small round blue cell tumor of childhood, probably rhabdomyosarcoma (and I had never heard of a sarcoma - and neither had my parents), a very rare and aggressive form of pediatric cancer. Further testing and staining revealed that I had alveolar rhabdomyosarcoma, with a PAX3-FOXO1 fusion. Additional genomic testing showed that my tumor cells also carried CDK4 amplification. I was told I had stage 3 disease and a 30 percent chance of survival.
As a freshman in college, I had thought that I was on my way to being an adult and was looking toward my future. Instead, I learned that I had this incredibly rare and deadly form of cancer. It was all very ironic to me, too, that I was too old for the pediatrician, yet I had a rare and aggressive pediatric cancer. Furthermore, I had been volunteering at Children's Healthcare of Atlanta all the while this tumor was forming and growing inside me, and I returned to CHOA not as a volunteer, but as a cancer patient. I was thrown into this terrifying world of baldness and sickness and chemotherapy and radiation protocols and statistics and....death.
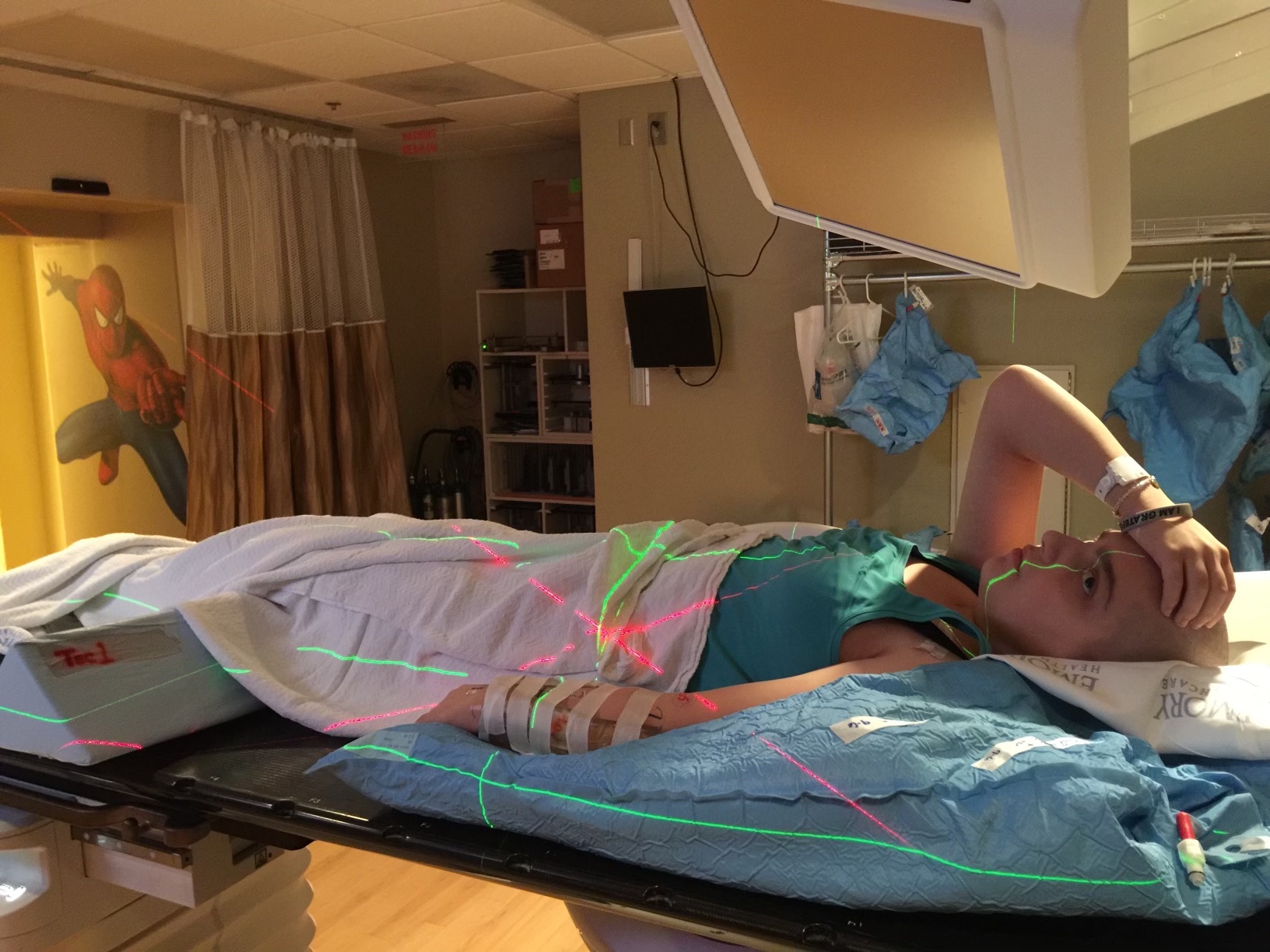 (Photo Provided)
(Photo Provided)
I endured a 43-week intensive treatment protocol. I was on the VAC/VI regimen - 14 cycles of chemotherapy consisting of four different drugs. Sometime during this I had a "chemo holiday” to have surgical resection of the tumor and then resumed my chemotherapy. I had a total of 28 radiation treatments over 6 weeks to my forearm (for a total of 54 Gy of radiation). The treatment journey was painful and isolating. I lost all of my hair, which was very traumatic, and also a constant reminder that I was seriously ill. I was nauseous and bedridden most of the time. I developed third degree burns and open wounds on my arm from the radiation. I was constantly faced with imminent issues of life and death - I could die from the cancer, or from the brutal treatment.
In the end, I was very, very lucky. I finished my treatment protocol in March of 2017 and was declared to have No Evidence of Disease (NED). Since then, I have had 5 years of clear scans. I have collected a few new specialists and lifelong medications due to medical issues from the toxic treatments. But I am cancer free and the threat of relapse is much smaller at this stage. The surveillance will change now to primarily watching for secondary cancers that could develop from treatment.
These last 5 years "off treatment” have been very hard. They have been filled with lessons in learning how to live again. I am learning how to be grateful that I am alive while at the same time feeling such sorrow and guilt with the passing of each and every friend or child/teen/young adult I have come to know, especially those with my subtype and fusion. I had to learn how to manage the fears and anxieties that I continued to face. I had to learn how to mourn, but not be bitter, about what cancer has taken from me. I had to learn how to live with hope - hope that I would continue to live, and if I didn't, hope that that would somehow be okay, that I would be ready, if and when the time came.
 (Photo Provided)
(Photo Provided)
When I was newly diagnosed and beginning treatment, I longed for the day I was finished and vowed to get as far away from this cancer world as I could. However, as I finished treatment, I was lost. I felt like I was a completely different person. It felt like my old world had gone on without me. It was difficult to relate to people and their mundane concerns. I had made new friends, only to see them die and their families suffer. And I was shocked and angry to learn that there was little funding for childhood cancers and especially for sarcomas in general, as they are rare, yet devastating. The chemotherapies in my protocol were decades old. It was around this time that I was introduced to Rally Foundation for Childhood Cancer Research, and Rally provided me a community of support and offered me opportunities to share my story at events to raise awareness and research funds. In September of 2017, I attended CureFest, a national annual event in Washington, D.C. that brings together the childhood cancer community, the public, and the scientific and medical community to advocate for pediatric cancers. At CureFest, Rally Foundation invited me to speak at the kick off ceremony to a crowd of over 400 people. I attended a rally marching through the streets of D.C. to the Capitol; participated in a candle light vigil in front of the White House; worked in the Rally Foundation booth to welcome visitors and to explain the foundation's mission; and represented Rally Foundation in joining Kids v Cancer to learn about legislation for childhood cancer. I found this advocacy work to be therapeutic and empowering. It gave me a sense of meaning and purpose. It also seemed like the right thing to do. Later that month, I participated in Rally Foundation's September campaign and personally raised over $3,000 to fund research. In 2018, I spoke at a luncheon in connection with Rally's big spring fundraiser and felt that I made a difference. In 2019, I became a Rally Kid Coordinator Intern and loved being on the inside of this amazing organization and cause. At the conclusion of my internship, Rally nominated me to apply for the DOD Peer-Reviewed Cancer Research Program for rare pediatric, adolescent, and young adult (AYA) sarcomas. I was thrilled and honored to be invited to be the PRCRP consumer reviewer on this DOD sarcoma panel.
The 2021 panel was conducted in a virtual setting due to the pandemic. I had developed a high interest in young adult sarcomas and had already acquired quite a bit of general knowledge. This was an opportunity to learn even more and to share my experience with the team as well as having the opportunity to learn about the research and new developments that were happening with sarcomas. I enjoyed the analysis and appreciated the feedback and assistance from my Scientific Review Officer. I loved the interaction from the scientific community members on the panel and felt they all valued and appreciated my role and what I had to offer from my consumer perspective. I learned so much about the process and thoroughly enjoyed the experience and felt a part of the team. It was truly an amazing experience. Next, I had the opportunity to serve on an AYA cancer panel as the consumer member. It was fulfilling to review a new set of applications with a new team and to be involved with other forms of AYA cancers, not just sarcomas. After I had struggled a bit with one particularly technical application and put in a lot of time, my Scientific Review Officer kindly reached out to me and reminded me that as a consumer reviewer, I was not expected to completely understand the highly technical components of the applications, but rather to offer insights from my personal experience as a cancer patient and survivor. He thanked me for this valuable perspective, which put me at ease and helped me feel like an important part of the team. Again, I felt guided, encouraged, supported and appreciated in offering my experiences and viewpoint. On another note, I am extremely grateful for the critical contributions that the DOD is making toward these rare and underfunded cancers and this overlooked group. Also, to add, both of my grandfathers served in the military, so it is very meaningful to me to be a part of this process, even in my small capacity.
In December of 2021, I graduated from college with a Bachelor's of Science in Human Development. I accepted a position working in an urgent care setting as patient service representative, while I pursue the next steps required to become a Certified Child Life Specialist. My dream is to work with children, teens and adolescents on the cancer floor. I also plan to continue my advocacy work in cancer research and I very much look forward to continuing to be a part of the PRCRP application review panels.
The views, opinions, and/or findings contained in this paper are those of the author(s) and should not be construed as an official Department of Defense or Department of the Army position, policy, or decision.
Last updated Wednesday, September 17, 2025
 An official website of the United States government
An official website of the United States government
 ) or https:// means you've safely connected to the .mil website. Share sensitive information only on official, secure websites.
) or https:// means you've safely connected to the .mil website. Share sensitive information only on official, secure websites.
