Breast Cancer
Death Effector Domain-Containing Protein (DEDD) Vulnerability to Cell Cycle Inhibition in Triple-Negative Breast Cancer (TNBC)



Posted July 22, 2020
Siyuan Zhang, Ph.D., University of Notre Dame

The identification of therapeutically targetable biomarkers has revolutionized the treatment of ER+ and HER2+ breast cancers. Unfortunately, for patients diagnosed with TNBC, the most aggressive and clinically challenging subtype to treat, molecular biomarkers that can be therapeutically targeted remain elusive. Although a large percentage of TNBCs express epidermal growth factor receptor (EGFR), clinical trials using EGFR inhibitors, such as lapatinib, have not shown promise, suggesting alternative survival mechanisms that facilitate TNBC proliferation under EGFR inhibition. With a Fiscal Year 2017 Breast Cancer Research Program Breakthrough Award – Funding Level 2, Dr. Zhang’s laboratory explored alternative pathways that allow TNBC cells to adapt to inhibition of the EGFR pathway, with implications for potential therapeutic targets that, when inhibited, synergize with EGFR inhibitors and render TNBC susceptible to treatment.
As recently published in Nature Communications, through a whole genomic synthetic lethal screening, Dr. Zhang’s research team identified DEDD, a protein normally localized to the nucleus of cells that promotes the activation of cell death pathways, as a mediator of TNBC cell proliferation. Specifically, the nuclear-to-cytosolic transition and overexpression of DEDD in lapatinib-treated TNBC cell lines contributed to cell cycle progression by promoting the degradation of the retinoblastoma (Rb) tumor suppressor protein via the CDK4/6/Rb pathway. Because CDK4/6 and Rb are critical drivers of normal cell cycle progression, these results suggested that DEDD has distinct tumor-promoting roles in the cytosol of TNBC cells, which are independent of its known nuclear function.
Dr. Zhang and his team hypothesized that DEDD’s cell cycle-promoting role in TNBC cells represented a tumor-specific vulnerability for therapeutic targeting, potentially in combination with other cell cycle progression proteins such as CDK4 and CDK6. Recently, three CDK4/6 inhibitors received U.S. Food and Drug Administration (FDA) approval for treating ER+ breast cancer: albociclib, ribociclib, and abemaciclib. Rb is the major target of CDK4/6 phosphorylation, and the current consensus is that CDK4/6 inhibition prevents degradation of Rb and restores its tumor suppression activity. Patients with mutated or absent Rb, such is the case for the majority of TNBC patients, are therefore excluded from clinical trials of these therapeutics. To determine whether cytoplasmic DEDD expression could lead to increased sensitivity to CDK4/6 inhibition, the researchers evaluated TNBC cell proliferation in vitro following single or combination treatment. Interestingly, targeting CDK4/6 in combination with lapatinib in DEDD-overexpressed TNBC cells significantly and synergistically inhibited cell proliferation. Importantly, the synergistic response was independent of Rb expression levels.
The team next translated their findings to a treatment setting by examining DEDD expression and localization, as well as drug sensitivity, in both cell line- and patient-derived xenograft mouse models of TNBC. Initial tumor immunohistochemistry analyses showed that DEDD predominantly localized to the cytoplasm of tumor cells. Treating TNBC mouse tumors with either lapatinib or CDK4/6 inhibitors alone did not result in a reduction in tumor size or proliferation index. However, combination therapy led to significant reductions in both the size and proliferation index of tumors across all models. Importantly, TNBC tumors that were highly resistant to lapatinib treatment alone and moderately responsive to treatment with a CDK4/6 inhibitor were sensitive to combination treatment, as evidenced by significantly reduced tumor size, reduced proliferation, and increased tumor cell death.
This research challenges current dogma that CDK4/6 inhibitors are only effective in breast cancer tumors expressing wild-type Rb protein. Rb expression is currently a requirement for the use of CDK4/6 inhibitors clinically. As a result, most TNBC patients are not treated with CDK 4/6 inhibitors or included in current CDK4/6 inhibitor clinical trials since Rb loss is common in TNBC. The results of this study provide the first proof-of-concept supporting the use of FDA-approved CDK4/6 inhibitors in TNBC tumors overexpressing DEDD, regardless of whether or not the tumor expresses wild-type levels of Rb. Since the majority of TNBC tumors overexpress DEDD, this implies that many existing TNBC patients could benefit from these existing therapies that are already approved for ER+ breast cancer and currently being tested in other indications. This study provides preclinical rationale for the initiation of clinical trials testing the efficacy of these inhibitors in TNBC patients, using cytoplasmic DEDD expression as a patient selection guideline.
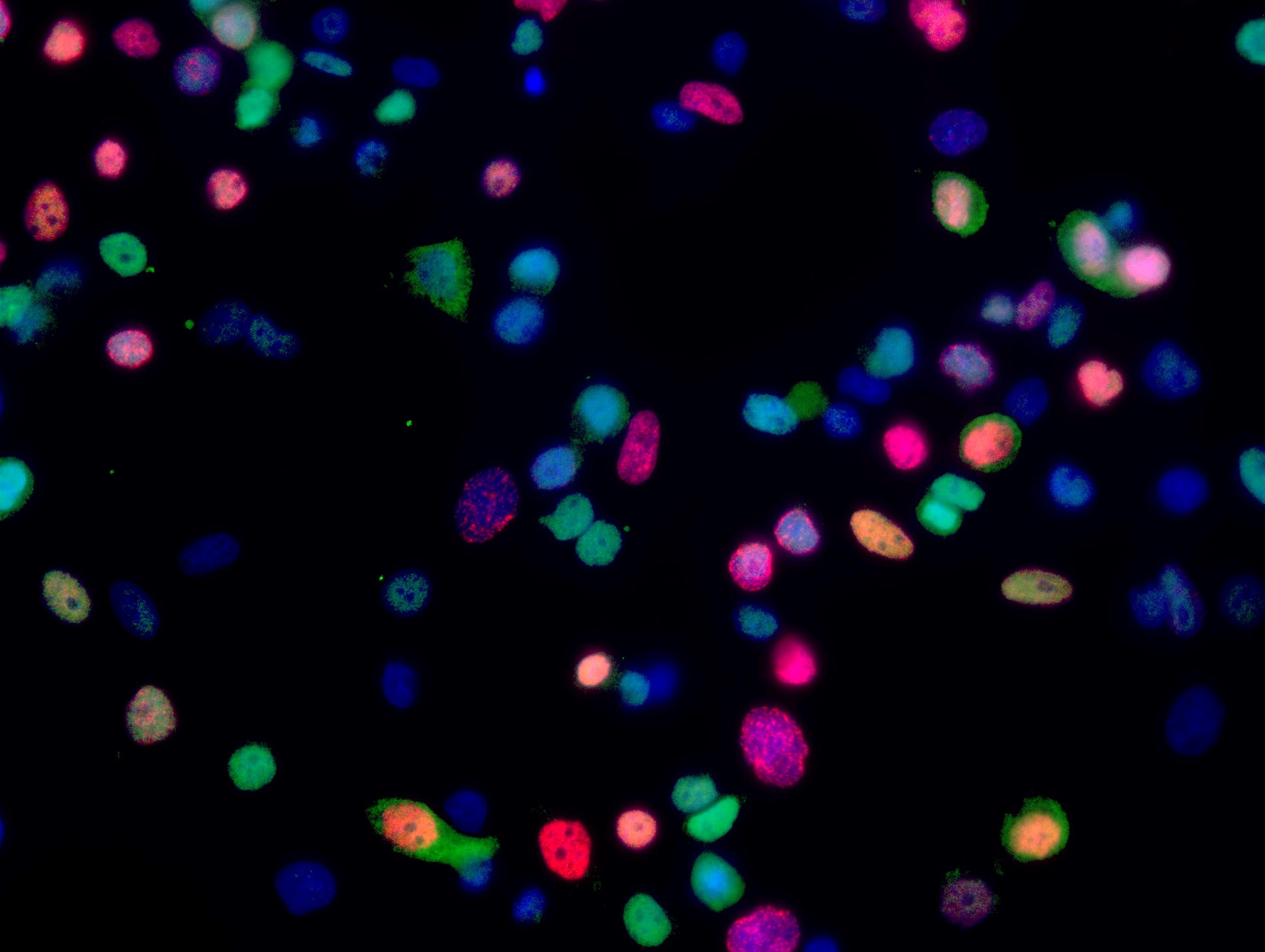
DEDD intracellular location and its association with cell cycle progression were assessed by immunofluorescence staining. Cell proliferation is indicated by EdU (Red) incorporation into the nucleus (blue). DEDD expression was detected anti-DEDD IF staining (green)
Publication:
Ni Y, Schmidt KR, Werner BA, et al. 2019. Death effector domain-containing protein induces vulnerability to cell cycle inhibition in triple-negative breast cancer. Nature Communications 10(1):2860.
Link:
Last updated Thursday, November 6, 2025
 An official website of the United States government
An official website of the United States government
 ) or https:// means you've safely connected to the .mil website. Share sensitive information only on official, secure websites.
) or https:// means you've safely connected to the .mil website. Share sensitive information only on official, secure websites.
