Breast Cancer
Identification of Actionable Networks Promoting Breast Cancer Progression and Brain Metastasis



Posted January 12, 2024
Ann Marie Pendergast, Ph.D., Duke University School of Medicine
 Dr. Ann Marie Pendergast
Dr. Ann Marie Pendergast
(Photo Provided)
Metastasis is the spread of cancer cells from the initial tumor site to another location of the body. For those living with breast cancer,
With funding from a fiscal year 2017 (FY17) Breakthrough Award Funding Level 2, Dr. Ann Marie Pendergast and her team conducted research on ABL kinase inhibition in a mouse model of HER2+ BCBM and evaluated the effect on breast cancer progression and metastasis to help clarify its relationship with HER2. In mice treated with an inhibitor of ABL kinase, there was an 80% decrease in ABL kinase activity, decreased metastasis to the brain, and increased overall survival as compared to controls. These results were replicated and confirmed in several HER2+ brain metastatic cell lines, including a mouse model with a functional immune system, demonstrating that treatment with an ABL kinase inhibitor approved by the U.S. Food and Drug Administration (FDA) for other cancer types also inhibited brain metastases.
 Dr. Ann Marie Pendergast’s research team. From left to right: Dr. Courtney M. McKernan,
Dr. Ann Marie Pendergast’s research team. From left to right: Dr. Courtney M. McKernan,
To understand the relationship of ABL and HER2, the investigators evaluated HER2 protein levels in three BCBM cell lines and observed that the inhibition of ABL kinase led to a reduction in HER2 protein, indicating a relationship between the ABL kinase and HER2 protein expression. Pendergast and her team tested whether ABL kinase inhibition altered ERBB2 transcription, HER2 protein stability, and/or translation of the corresponding messenger RNA (mRNA) into protein. Pharmacologic and genetic inhibition of ABL kinases resulted in little to no change in ERBB2 mRNA levels and did not affect HER2 protein stability. Rather, ABL kinase inhibition or depletion profoundly decreased HER2 protein levels by impairing ERBB2 mRNA translation, leading to a decrease in HER2 protein expression. RNA binding proteins, such as Y-box-binding protein 1 (YB-1), play an important role in regulation of protein synthesis by binding the mRNA. Interestingly, upon ABL kinase inhibition, Dr. Pendergast found the decline in HER2 protein levels was due to a decreased interaction between YB-1 and the HER2/ERBB2 mRNA. Further evaluation confirmed that reduced YB-1 expression resulted in a decreased number of HER2 proteins and a dramatic reduction of cell viability thus providing evidence that YB-1 is involved in HER2 regulation. Notably, the team found that loss of YB-1 expression in HER2+ breast cancer brain metastatic cells decreased HER2 protein levels and impaired brain metastatic outgrowth leading to improved survival in preclinical models.
To further understand the mechanistic relationship between ABL, YB-1, and HER2, the team conducted experiments assessing phosphorylation, a molecular process that governs protein activity and stability. The team found that ABL activity leads to YB-1 phosphorylation. This, in turn, revealed that ABL-mediated phosphorylation of YB-1 is required to promote HER2 protein synthesis. This discovery — ABL-YB-1 signaling, its control of HER2 protein synthesis, and the potential to treat HER2-driven brain metastases through inhibition of ABL — opens up a promising new therapeutic target mechanism.
While previous studies have examined HER2 overexpression regulation in tumors, the Pendergast team’s explorations of the cellular mechanisms behind HER2 protein synthesis, specifically in the context of brain metastasis, provide evidence for the mechanism of ABL-YB-1 signaling and its effects on the HER2 protein. The discovery that cancer cells expressing HER2 can be targeted by BBB-permeable ABL kinases, one of which is FDA-approved for other cancer types, suggests these drugs might be effective in treating HER2+ BCBM. Continued research on the ABL-YB-1 pathway and its regulation of HER2 may ultimately improve breast cancer treatment and decrease the development of metastasis, thereby improving patient outcomes.
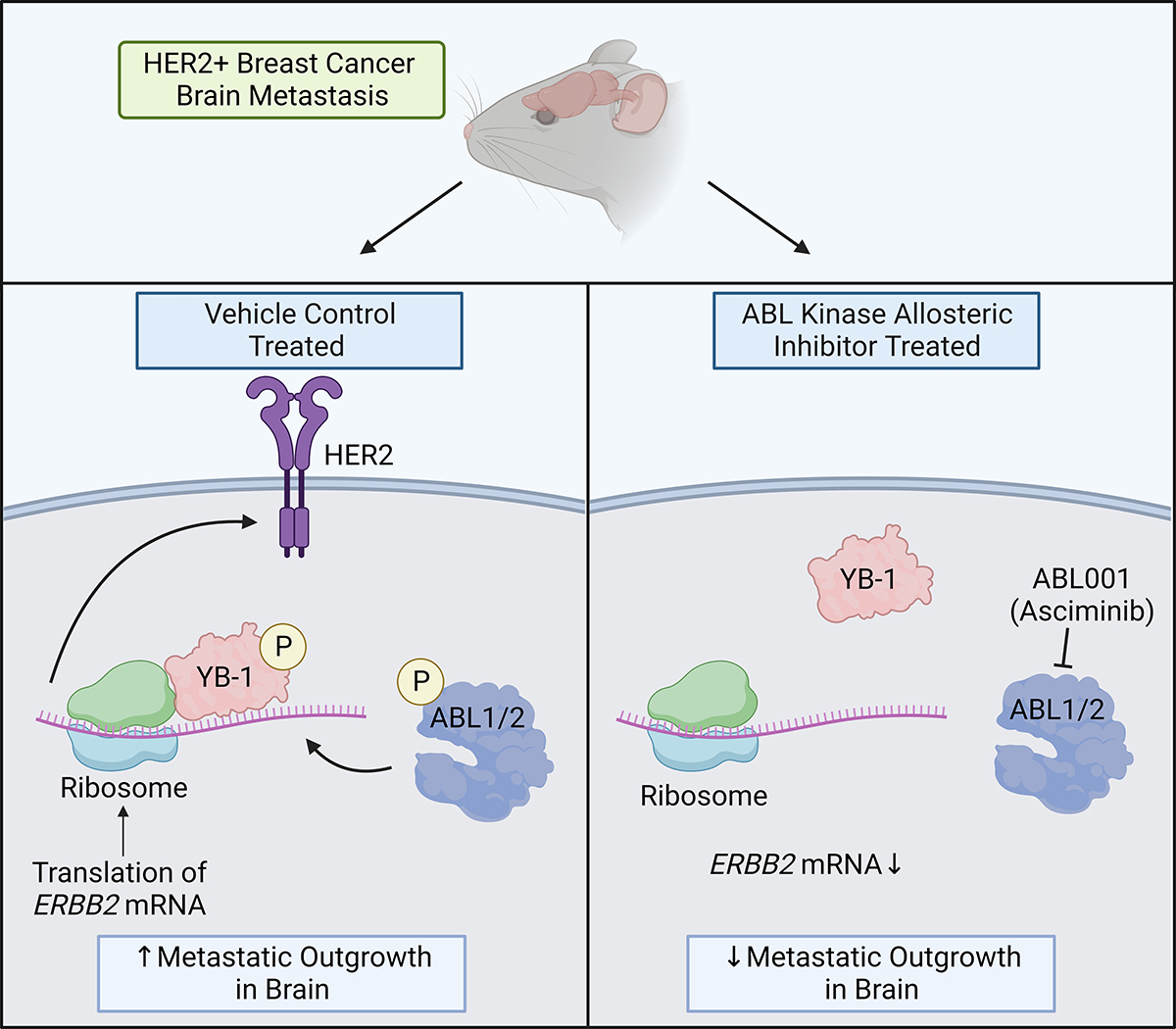 Figure 1 illustrates the role of the signaling axis between the Abelson (ABL) kinase and
Figure 1 illustrates the role of the signaling axis between the Abelson (ABL) kinase and
(Figure provided. Image prepared by Hannah Thrash, Duke University.)
References:
1American Cancer Society. Survival Rates for Breast Cancer. Last revised 3/1/2023. https://www.cancer.org/cancer/types/breast-cancer/understanding-a-breast-cancer-diagnosis/breast-cancer-survival-rates.html.
Publications:
McKernan CM, Khatri A, Hannigan M, et al. 2022. ABL kinases regulate translation in HER2+ cells through Y-box-binding protein 1 to facilitate colonization of the brain.
Links:
Last updated Thursday, November 6, 2025
 An official website of the United States government
An official website of the United States government
 ) or https:// means you've safely connected to the .mil website. Share sensitive information only on official, secure websites.
) or https:// means you've safely connected to the .mil website. Share sensitive information only on official, secure websites.
