Peer Reviewed Orthopaedic
New Information in Our Understanding of Osteoarthritis Onset



Posted January 10, 2020
Tamara Alliston, Ph.D., University of California, San Francisco
Alexis Dang, M.D., Alfred Kuo, M.D., Ph.D., San Francisco Veterans Affairs Medical Center

Osteoarthritis (OA) affects more than 30 million Americans, causing pain and disability, and is the most common chronic joint disease worldwide. OA is an irreversible degradation of the joint-lubricating articular cartilage and surrounding tissues, for which no therapy exists beyond invasive joint replacement surgeries. Mechanical stress placed on joints is thought to contribute to the development of OA, and in extreme cases, these stresses or an acute injury may facilitate a more rapid, post-traumatic osteoarthritis (PTOA). PTOA presents a significant burden to the military as Service members develop complications with nearly twice the frequency of the civilian population and at a much younger age.
Recent studies have indicated that degenerative changes to subchondral bone, the thin surface of bone that lies directly beneath articular cartilage within the joint, may precede overlying cartilage degeneration and development of OA. Healthy bone requires the coordinated action of multiple cell types, including bone-embedded osteocytes. Osteocytes, or mature bone cells, are capable of local bone matrix resorption and deposition—a process called perilacunar/canalicular remodeling (PLR). Matrix-degrading enzymes, like matrix metalloproteinase-13 (MMP13), are secreted by osteocytes to initiate PLR, which maintains the integrity of lacunocanalicular network (LCN) within the bone. Proper maintenance of the LCN is critical to allow individual osteocytes to communicate and conduct the mechanosensory functions associated with normal healthy bones. However the role of PLR in subchondral bone, joints, or in the development of OA is unknown.
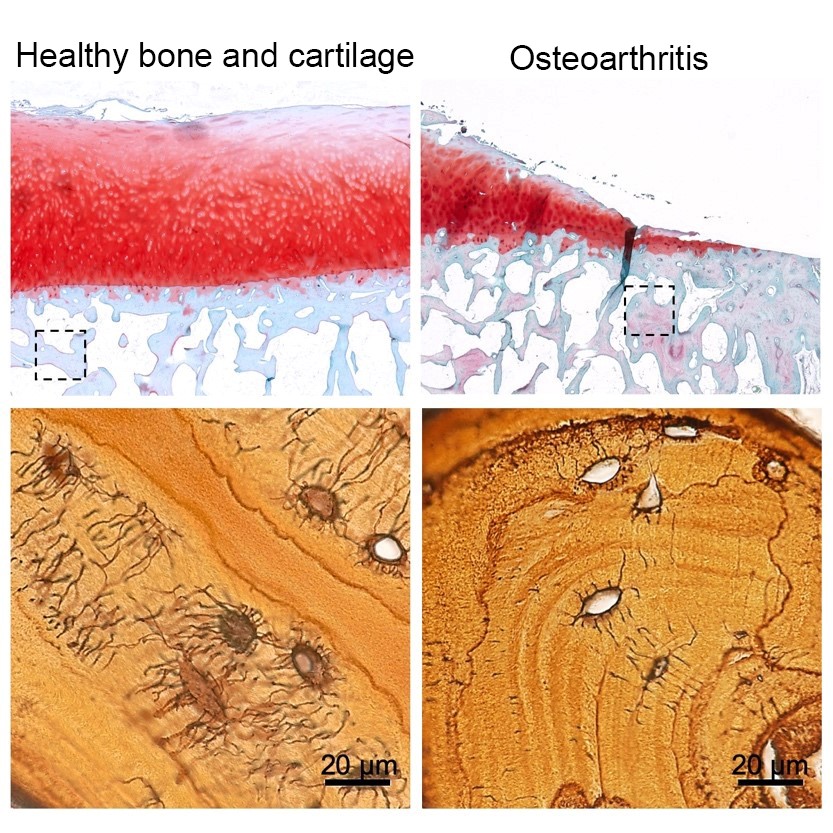
With a Fiscal Year 2013 Peer Reviewed Orthopaedic Research Program Idea Development Award, Dr. Tamara Alliston at the University of California, San Francisco, and her team investigated the role of subchondral bone and osteocyte-mediated PLR in the development of OA. The team’s work has been recently published in the prestigious journal, Bone Research. Five patients scheduled for total knee arthroplasty/replacement at the San Francisco Veteran Affairs Medical Center agreed and consented to donate their otherwise discarded surgically removed tissue. Dr. Alliston and her team analyzed the OA tissue in comparison to tissue without OA and established that patients with late-stage OA have demonstrable changes to their subchondral bone, including reduced LCN size, increased mineralization, and misaligned bone matrix fibers. These noted changes coincided with quantifiable reductions in several matrix-degrading enzymes that are important in PLR, including MMP13. The team also demonstrated that MMP13 production by osteocytes positively correlates with LCN area and length, suggesting that suppression of PLR also correlates with human OA.
To determine whether osteocytes and deregulated PLR are at the root of OA induction and not merely a consequence of the disease, Dr. Alliston’s group specifically deleted the MMP13 gene from otherwise normal osteocytes in a mouse model. The absence of MMP13 mimics deregulated PLR and OA-associated phenotypes in subchondral bone, including increased mineralization, significant reduction of the LCN, and modest alteration of matrix fiber alignment. Importantly, this deregulation of PLR led to an increase in OA-like articular cartilage degradation, suggesting that disruption of normal osteocyte function may induce the onset of OA. Within the articular cartilage of these MMP13 deficient mice, the team found evidence of OA marked by a change in the ratio of important cartilage matrix elements and an increase in the enzymes responsible for degradation.
Dr. Alliston’s work implicates for the first time a disruption in normal osteocyte biology as a primary event in the onset of OA. Changes to the subchondral bone in joints, mediated by deregulation of normal bone remodeling, appears capable of initiating the articular cartilage degeneration associated with OA. Restoring normal osteocyte function and PLR potentially represents an important new target to slow or stop a currently irreversible disease. The result of Dr. Alliston’s work advances the understanding of significant gaps in the knowledge of OA mechanisms associated with development of joint disease and could have a significant impact in advancing OA treatments for both Service members and the general public who are suffering from chronic joint disease.
Reference:
Link:
Last updated Monday, January 3, 2022

















